Public Health
Women’s Health: A Guide to Preventing Infections
- Sexually Transmitted Diseases
- Hepatitis
- Bacterial Vaginosis
- Vaginal Yeast Infections
- Urinary Tract Infections
- Safer Sex
- Colds
- Influenza (Flu)
- Pneumonia
- Vaccines
- Vaccines and Pregnancy
- Food Safety
- Food-borne Illness During Pregnancy
- Clean Hands
- Contact Lens Safety
- Definition of Terms
Sexually Transmitted Diseases
Sexually transmitted diseases (STDs) are infections that are spread by sexual contact with someone who has an STD. STDs are mostly spread through vaginal, anal, or oral sex, and genital touching.
There are about 19 million new STD infections each year in the United States. There are over 20 types of STDs. STDs may be caused by bacteria, parasites, or viruses. STD infection may show a range of signs, or no signs at all. Sometimes people have an STD and don't know it. The only way to know if you have an STD is by a medical exam and testing by your health care provider.
Common STDs caused by bacteria that can be treated and cured with antibiotics include:
- Chlamydia
- Gonorrhea
- Syphilis
Common STDs caused by viruses that can be controlled with treatment include:
- Hepatitis
- Herpes
- HIV
- HPV
If you have an STD, tell current and recent sex partners of the infection.
How do you know if you have an STD?
Your health care provider can examine and test you for STDs. Some women are at a higher risk for STDs. They should have regular exams and testing. Higher risk women include those who:
- Have had a previous STD
- Have new or multiple sexual partners
- Use condoms only some of the time
- Have sex for drugs or money
- Use needles for illegal drugs
Using condoms or not having sex are the best options to protect yourself from STDs.
How can women avoid STDs?
- Avoid sexual contact.
- Including vaginal, anal, or oral sex, or genital touching.
- This is the only way to be absolutely sure of avoiding STDs.
- Have safer sex:
- Reduce the number of sexual partners.
- Use barriers, including:
- Male condom
- Female condom
- Condoms, when used correctly, can
reduce the risk of getting an STD. Each
time you have sex use a condom (male or
female type):
- Before vaginal sex
- Before anal sex
- Before oral sex
- Condoms, when used correctly, can
reduce the risk of getting an STD. Each
time you have sex use a condom (male or
female type):
- Dental dam
- Plastic wrap, if other barriers are not available
- Have sex with only one partner who does not have sex with others and does not have an STD.
- Know that washing the vagina or douching after sex will not prevent it.
- The American Congress of Obstetricians and Gynecologists (ACOG) recommend that women do not douche.
- Douching can change the balance of germs and acidity in a healthy vagina.
- Any changes in that balance can cause an over growth of bad bacteria. This can lead to a yeast infection or bacterial vaginosis.
- If you have a vaginal infection, douching can push infection-causing bacteria up into the uterus, fallopian tubes, and ovaries. This can cause more serious problems.
For more information, see Safer Sex.
What about pregnancy?
Some STDs can also be passed on to the baby during pregnancy, birth, or breastfeeding.
It is important for all pregnant women to be tested for STDs. Treatment of STDs can prevent the effects of the STD on the baby. If you are pregnant or breastfeeding and have an STD, you should talk to your health care provider about the risk of passing the STD to your baby.
Some STDs can cause:
- Early birth
- Low birth weights
- Other severe problems in the newborn baby
For more on STDs
- Centers for Disease Control and Prevention (CDC):
- U.S. Department of Health and Human Services (HHS), Office on Women's Health:
Chlamydia
Chlamydia is an infection caused by bacteria. It is the most commonly reported sexually transmitted disease (STD) in the United States.
How is it spread?
Women get chlamydia through vaginal, oral, or anal sexual contact with an infected person.
What are signs of chlamydia in women?
75% of infected women and 50% of infected men have no signs. Signs in women include:
- Increased or unusual vaginal discharge
- Burning with urination
- Pain in the back or abdomen
- Nausea
- Fever
- Discomfort during sex
- Bleeding between periods
- Rectal pain, bleeding, or discharge
- Sore throat
Most women with chlamydia do not show any signs of infection.
How do you know if you have chlamydia?
The only way to know if you have chlamydia is by a medical exam. Most women with chlamydia do not have any signs of infection. See your health care provider to be tested for chlamydia each year if you:
- Are age 25 or younger and are sexually active
- Are older than 25 with new or multiple sex partners
- Do not practice safe sex
- Are having sex with someone who might be having sex with others
- Are pregnant
How is it treated?
Chlamydia can be treated and cured with antibiotics. Always finish antibiotic treatment, even if signs of chlamydia go away. Do not have sex until after treatment and signs of it are gone. See your health care provider if your signs do not go away after finishing treatment.
What can happen if you have chlamydia for a long time?
- Problems getting pregnant
- Pregnancy outside of the uterus
- Swelling in the anus
- Eye and joint redness and pain
- More likely to get HIV from a partner who is infected with HIV
If you have chlamydia
- Always finish all antibiotic treatment.
- Do not have sex with someone who has chlamydia or has not finished treatment (to prevent re-infection).
- Tell current and recent sex partners of the infection so they can get checked.
- Know that it can raise the risk of getting and spreading HIV.
How can you avoid chlamydia?
- Avoid sexual contact.
- Have safer sex:
- Reduce the number of sexual partners.
- Condoms, when used correctly, can reduce the
risk of getting chlamydia. Each time you have sex
use a condom (male or female type):
- Before vaginal sex
- Before anal sex
- Before oral sex
- Have sex with only one partner who does not have sex with others and does not have chlamydia.
- Know that other forms of birth control do not protect against chlamydia.
For more information, see Safer Sex.
What about pregnancy?
All pregnant women should be tested for chlamydia. If you are pregnant and have chlamydia, you should discuss your pregnancy and infection with your health care provider. Pregnant women with chlamydia can have early births or babies with eye and lung infections.
Pregnant women with chlamydia can pass it to their babies during childbirth.
For more on chlamydia
- Centers for Disease Control and Prevention (CDC): Chlamydia – CDC Fact Sheet
- U.S. Department of Health and Human Services (HHS), Office on Women's Health: Chlamydia Fact Sheet
- U.S. National Library of Medicine: Chlamydia Infections in Women
Genital Herpes
Genital herpes is a sexually transmitted disease (STD) caused by herpes simplex viruses. Many people with herpes have no signs of infection and do not know they have it.
There are 2 herpes simplex viruses that can cause infection
- One causes most genital herpes.
- The other virus can also cause genital herpes but more often causes blisters of the mouth and lips (e.g., cold sores or fever blisters).
The U.S. Centers for Disease Control and Prevention (CDC) states that about 1 out of 6 people ages 14 to 49 have genital herpes.
Women are more easily infected with herpes than men.
How is it spread?
The herpes virus is spread by skin-to-skin contact with a person who has the herpes virus:
- Most often, from herpes sores or blisters
- Less often, from normal looking skin where the virus first entered the body
- During vaginal, anal, or oral sexual contact, or skin-to-skin contact. This may happen even without visible sores.
- The herpes virus enters the body through the:
- Lining of the mouth
- Labia
- Vagina
- Regular skin that has small cracks or cuts
People with a weak immune system can get a herpes infection more easily. A weak immune system is caused by some diseases (e.g., cancer, HIV/AIDS) and by some medicines used to treat serious diseases.
People who don't know they have herpes can still spread the virus to others.
What are signs of genital herpes in women?
Women who have the herpes virus may have no outbreaks or signs of infection. Many do not know they have the virus. Once you are infected, the virus stays in your nerve cells for life. When the virus is not active, there is no sign of infection. When the virus becomes active, a herpes outbreak occurs. Some women may not have any outbreaks or may have only one outbreak, while others may have multiple outbreaks.
First Outbreak
The first herpes outbreak often occurs within the 2 weeks after contracting the virus from an infected person. The first signs may include:
- Itching, tingling, or burning feeling in the vaginal or anal area
- Flu-like symptoms, including fever
- Swollen glands
- Pain in the legs, buttocks, or vaginal area
- A change in vaginal discharge
- Headache
- Painful or difficult urination
- A feeling of pressure in the area below the stomach
After a few days, painful sores, blisters, or ulcers may develop where the virus entered the body. These areas include:
- The vaginal or anal area
- The mouth
- Inside the vagina
- On the cervix
- In the urinary tract
- On the buttocks or thighs
- On other parts of your body where the virus has entered
Sometimes the first outbreak will not occur until months or years after infection.
Other Outbreaks
After the first outbreak, you may have more outbreaks. For most, these outbreaks occur less often over time. The signs of herpes infection are usually milder than during the first outbreak, and they go away faster.
For people with a weak immune system, outbreaks can be severe and long-lasting.
See your health care provider to be tested if you have signs of herpes.
How do you know if you have genital herpes?
The only way to know if you have genital herpes is by a medical exam. Your health care provider can examine you and test for it. Lab samples are taken from a sore, blister, or blood. Your health care provider may ask to test you for other infections at the same time.
Tell current and most recent sex partners of your herpes infection.
How is it treated?
Genital herpes can be treated, but it cannot be cured. Anti-viral medicines can make outbreaks:
- Shorter
- Less severe
- Less frequent
Living with genital herpes causes some people to:
- Feel embarrassed or ashamed
- Worry about infecting a sexual partner
- Worry that having herpes will affect relationships with sexual partners
- Avoid dating or sexual relationships
Most people with herpes are able to live with the virus and manage their outbreaks. Talking to trusted health care providers and friends can help. Your health care provider can talk to you about medicines that treat outbreaks and about ways to reduce the chance of passing the virus on to a sexual partner.
Medicines can help lower the chance that you will pass the virus to others.
If you have genital herpes, during outbreaks you should
- Keep the infected area clean and dry.
- Avoid touching the sores or blisters.
- Clean hands after contact with the infected area.
- Avoid skin-to-skin contact from the time you first notice signs of herpes until the sores have healed.
For more on how to clean hands, see Clean Hands.
How can you avoid genital herpes?
Most women get genital herpes through sexual contact with a person who has herpes sores. You can get the virus without having sex. To avoid infection:
- Avoid skin-to-skin and sexual contact.
- Have safer sex:
- Reduce the number of sexual partners.
- Condoms, when used correctly, can reduce the
risk of getting genital herpes. Each time you have sex
use a condom (male or female type):
- Before vaginal sex
- Before anal sex
- Before oral sex
- Have sex with only one partner who does not have sex with others and does not have herpes.
- Know that other forms of birth control do not protect against herpes infection.
For more information, see Safer Sex.
What about pregnancy?
A pregnant woman who has genital herpes can pass the virus to her baby. A baby born with herpes might:
- Be born early
- Have brain, skin, or eye problems
- Not survive
If you are pregnant, you should tell your health care provider if you have herpes. If you show any signs of herpes during pregnancy, tell your provider. Pregnancy can be managed safely if your health care provider knows about your herpes. Medicines can help babies born with herpes if they are treated right away.
For more on genital herpes
- Department of Veterans Affairs (VA): Herpes Simplex Virus
- Centers for Disease Control and Prevention (CDC): Genital Herpes – CDC Fact Sheet
- U.S. Department of Health and Human Services (HHS), Office on Women's Health: Genital Herpes Fact Sheet
Genital Warts
Genital warts are caused by low-risk types of human papillomavirus (HPV). These viruses may not cause warts in everyone.
How are they spread?
Women can get genital warts from sexual contact with someone who has HPV. Genital warts are spread by skin-to-skin contact, usually from contact with the warts. It can be spread by vaginal, anal, oral, or handgenital sexual contact. Genital warts will spread HPV while visible, and after recent treatment. Long-term sexual partners usually have the same type of wart-causing HPV.
What are signs of genital warts in women?
Genital warts can grow anywhere in the genital area:
- In the vagina
- Around the vaginal opening
- On the cervix (the opening to the womb)
- On the groin
- In or around the anus
- In the mouth or throat (rare)
Genital warts:
- Can be any size – from so small they can't be seen, to big clusters and lumps
- Can be smooth with a "mosaic" pattern or bumpy like a cauliflower
- Are soft, moist and flesh-colored
- Can cause itching, burning or pain
Not all HPV infections cause genital warts. HPV infections often do not have any signs that you can see or feel. Some HPV infections can be more serious, see HPV.
Even if you can't see any genital warts, you could still have an HPV infection.
How do you know if you have genital warts?
Genital warts can be detected by:
- Yourself
- A sexual partner
- A health care provider
The only way to confirm HPV infection is if your health care provider does an HPV test.
How is it treated?
See your health care provider to discuss treatment. Even when genital warts are treated, the HPV infection may remain. Warts may also return after treatment. Over-the-counter treatments for other types of warts should not be used. Treatments for genital warts include:
- Watch and wait to see if the warts stay the same, get bigger, or go away
- Medicines applied directly to the warts. These can include prescribed creams.
- Burning off the warts
- Freezing off the warts
- Cutting the warts out
- Using special lights or lasers to destroy the warts.
What can happen if you have genital warts for a long time?
The immune system fights HPV infection. The types of HPV that cause genital warts do not cause cancer. Without any treatment, genital warts may:
- Go away
- Remain unchanged
- Increase in size or number
If you have genital warts
- Discuss treatment for genital warts with your health care provider.
- Know that it you may never know when you got HPV or who gave it to you.
- Know that partners that have been together for a while often share the same HPV types, even if both have no symptoms.
Condoms may not fully protect against HPV since HPV can infect areas not covered by a condom.
How can you avoid genital warts?
- Get vaccinated against HPV.
- Certain types of HPV vaccines protect against the low-risk HPV that causes 90% of genital warts.
- HPV vaccine is safe for all females 9 to 26 years old.
- The Centers for Disease Control and Prevention (CDC) recommends all 11-12 year old girls get the HPV vaccine.
- Avoid sexual contact.
- Have safer sex:
- Reduce the number of sexual partners.
- Condoms, when used correctly, can reduce the
risk of getting HPV. But, condoms may not cover
all infected areas. Each time you have sex
use a condom (male or female type):
- Before vaginal sex
- Before anal sex
- Before oral sex
- Have sex with only one partner who does not have sex with others and does not have HPV.
- Know that other forms of birth control do not protect against HPV.
For more information, see Safer Sex.
What about pregnancy?
Genital warts rarely cause problems during pregnancy and birth. Most women who no longer have visible genital warts do not have problems with pregnancy or birth. If you are pregnant, you should discuss treatment options with your health care provider as the warts may:
- Grow larger and bleed
- Make it difficult to urinate if growing in the urinary tract (rare)
- Make the vagina less elastic during birth if the warts are in the vagina (rare)
- Cause a need for a cesarean section (C-section) birth if the warts block the birth canal (rare)
- Be passed to the baby during birth (rare)
For More on Genital Warts
- Centers for Disease Control and Prevention (CDC):
- U.S. Department of Health and Human Services (HHS), Office on Women's Health: Human Papillomavirus (HPV) and Genital Warts Fact Sheet
Gonorrhea
Gonorrhea is an infection spread by bacteria. Also known as "the clap" or "the drip", it affects both women and men. Women can get it in moist, warm areas such as the vagina, reproductive organs, anus, mouth, throat, and eyes.
How is it spread?
Women get gonorrhea from sexual contact with someone who is infected. Anyone who has gonorrhea can spread it to others. Gonorrhea can be spread through oral, vaginal, and sexual contact between:
- Men and women
- Women and women
- Men and men
What are signs of gonorrhea in women?
Some women and men can have gonorrhea without any signs. For women, signs include:
- Painful or burning urination
- Increased vaginal discharge
- Bleeding between periods or after sex
- Vaginal itching and irritation
- Discomfort or pain during sex
- Urgent or increased need to urinate
- Anal discharge, pain, bleeding or itching
- Fever, abdominal pain, rashes, and swelling or pain in joints over time
- Sore throat
- Red or itchy eyes
- Eye discharge
See your health care provider to be tested if you have signs of gonorrhea.
Women can get or spread HIV more easily if they have gonorrhea.
How do you know if you have gonorrhea?
The only way to know if you have gonorrhea is by a medical exam. Your health care provider can examine you and test for it. Lab samples may be taken from the vagina, bladder, bowels, throat, urine, or eyes. Your health care provider may ask to test you for other infections at the same time. See your health care provider to be tested for gonorrhea each year if you:
- Are age 25 or younger and are sexually active
- Are older than 25 with new or multiple sex partners
- Do not practice safe sex
- Are having sex with someone who might be having sex with others
- Are pregnant
Get tested for gonorrhea if your sex partner has it.
How is it treated?
Gonorrhea can be treated and cured with antibiotics. Always finish antibiotic treatment, even if signs of gonorrhea go away. Do not have sex until after treatment and signs of it are gone. See your health care provider if your signs do not go away after finishing treatment.
What can happen if you have gonorrhea for a long time?
Some women have no signs of gonorrhea until they are very sick and have permanent damage to their health. If untreated, gonorrhea can cause severe problems that include:
- Problems getting pregnant
- Pregnancy outside of the uterus
- Pain and infections in the abdomen
- The spread of gonorrhea to the blood, heart and joints
Tell current and most recent sex partners of the infection.
If you have gonorrhea
- Always finish all antibiotic treatment.
- Do not have sex with someone who has gonorrhea or has not finished treatment (to prevent re-infection).
- Tell current and recent sex partners of the infection so they can get checked.
- Know that it can raise the risk of getting and spreading HIV.
How can you avoid gonorrhea?
- Avoid sexual contact.
- Have safer sex:
- Reduce the number of sexual partners.
- Condoms, when used correctly, can reduce the risk of getting gonorrhea. Each time you have sex use a condom (male or female type):
- Before vaginal sex
- Before anal sex
- Before oral sex
- Have sex with only one partner who does not have sex with others and does not have gonorrhea.
- Know that other forms of birth control do not protect against gonorrhea.
For more information, see Safer Sex.
What about pregnancy?
Gonorrhea can cause miscarriages or early labor in pregnant women. If you are pregnant and have gonorrhea, you can pass the infection to your baby during birth. Your baby can have:
- Blindness
- Joint infections
- Blood infections
All pregnant women should be tested for gonorrhea. If treated, most problems in pregnancy and birth can be avoided.
Mothers who have gonorrhea can spread it to their own newborn babies.
For more on gonorrhea
- Centers for Disease Control and Prevention (CDC): Gonorrhea – CDC Fact Sheet
- National Institute of Allergy and Infectious Diseases (NIAID/NIH): Gonorrhea
- U.S. National Library of Medicine: Gonorrhea
- U.S. Department of Health and Human Services (HHS), Office on Women's Health: Gonorrhea Fact Sheet
HIV
HIV stands for human immunodeficiency virus. HIV is a virus that attacks and weakens the immune system. The immune system is the body's defense against infections.
If you are infected with HIV, you are said to be "HIV positive." Over time as HIV weakens your immune system, you are more likely to get other infections. The late stage of HIV infection is known as acquired immune deficiency syndrome (AIDS).
How is it spread?
Each year in the United States about 40,000 people get infected with HIV. The HIV virus is found only in certain body fluids:
- Blood
- Vaginal fluid
- Semen
- Breast milk
HIV is NOT spread by:
- Tears
- Sweat
- Feces
- Urine
Contact with infected body fluids can spread HIV. HIV is mostly spread by:
- Sexual contact:
- Vaginal and anal sex
- Sharing unclean sex toys
- Oral sex, very rarely
- Body fluids with HIV can enter tiny breaks or rips in the linings of the vagina, vulva, rectum, or mouth. Rips and tears in these areas can be common and often unnoticed.
- Needle sharing:
- Used or unclean needles
- During illegal drug use
- Breastfeeding:
- HIV can be spread to babies and others who drink breast milk from a woman who is HIV positive.
- Pregnancy and birth:
- HIV-positive women can spread the virus to their babies during pregnancy and birth.
HIV is rarely spread from a blood transfusion because:
- All donated blood is tested and screened for HIV.
- Blood and blood products that test positive for HIV are safely destroyed. None are used for transfusions.
- There is no risk of getting HIV when donating or giving blood.
VA offers HIV testing and treatment to all enrolled Veterans.
What are signs of HIV?
Most people with HIV will not show signs of HIV until years after infection. People who have been recently infected with HIV may have:
- Fever
- Chills
- Night sweats
- Headache
- Sore throat
- Swollen lymph nodes, usually on the neck
- Tiredness
- Rash
- Sores or infections in the mouth
- Body aches
You can't tell if a person is HIV infected by looking at them.
How do you know if you have HIV?
The only way to know you have HIV is by getting an HIV test. Routine HIV testing is recommended for all adults. HIV tests are offered by health care providers in doctor's offices, hospitals, local public health departments, and in community clinics. Most HIV tests use either blood or saliva. HIV tests are very accurate but may not show HIV from a recent infection. It is important to always discuss your test result and retesting with your test provider.
How is it treated?
There is no cure for HIV. But there are very effective treatments that help your body fight HIV. Your health care provider can help you decide when to start treatment and which medicines to take. Treatment is lifelong and can:
- Reduce the amount of virus in your body
- Reduce the spread of HIV to others
- Help most people with HIV live longer and healthier lives
The sooner you know if you have HIV, the sooner your provider can know if you need treatment.
What can happen if you have HIV for a long time?
If HIV infection is not diagnosed and treated, it can progress into AIDS. AIDS stands for acquired immune deficiency syndrome. AIDS is the late stage of HIV infection. When you have AIDS, the virus has severely weakened your immune system. If HIV is not treated, other life-threatening infections can occur. The only way to know if you have AIDS is through a medical exam and testing by your health care provider. Common signs of AIDS are:
- Rapid weight loss
- Fevers
- Night sweats
- Extreme tiredness
- Swelling of the lymph nodes in the armpits, groin, or neck which doesn't go away
- Diarrhea that lasts for more than a week
- Sores of the mouth, anus, or genitals
- Infections such as pneumonia, tuberculosis, and certain cancers
- Red, brown, pink, or purplish blotches on or under the skin or inside the mouth, nose, or eyelids
- Depression
- Memory loss and other brain or nerve problems
If you have HIV
- See a health care provider regularly.
- If on treatment, be sure to take medicines as prescribed.
- Tell current and recent sex partners that you have HIV.
- Avoid spreading HIV to others by:
- Using condoms during all sexual contact
- Not sharing used or unclean needles and sex toys
- Not breastfeeding
How can you avoid HIV?
The best ways to avoid HIV are:
- Avoiding sexual contact.
- Using condoms during all sexual contact.
- Not using or injecting illegal drugs. If you do use injection drugs, use a new sterile needle and clean drug equipment each time you prepare and inject drugs.
Other ways to reduce the risk of getting HIV include:
- Reducing the number of sex partners.
- Have sex with only one partner who does not have sex with others and does not have HIV.
- Knowing that douching or washing the vagina or anus after sex will not prevent HIV.
- Knowing that other forms of birth control do not protect against HIV.
- Not reusing or sharing needles, or drug equipment (works). If unused (new) needles and sterile drug equipment are not used, then all of it should be boiled in water or disinfected with a bleach solution, then rinsed with water before each use.
Ask your sex partners to test for HIV and other STDs.
For more information, see Safer Sex.
What about pregnancy?
A woman who has HIV can pass the virus to her baby during:
- Pregnancy
- Birth
- Breastfeeding
A woman with HIV who is not treated for HIV during pregnancy or labor has a 25% chance (1 in 4) of giving the virus to her baby. If the mother is treated, the chance of passing the virus to the baby is less than 2% (fewer than 2 out of 100 times). Babies born to HIV-positive mothers should be treated with anti-HIV drugs after birth.
If you are pregnant or want to get pregnant, you should:
- Get tested for HIV.
- Have your sexual partner tested.
- Discuss your HIV status with your health care provider.
- Talk to your health care provider about starting HIV treatment if you are HIV-positive.
- Take steps to avoid HIV by:
- Having safe sex. Each time you have sex use a condom.
- Not injecting illegal drugs.
- Not breastfeeding your infant if you have HIV.
If you are pregnant and HIV-positive, you should talk to your health care provider about starting treatment with anti-HIV drugs to prevent passing HIV to your baby.
For more on HIV/AIDS
- Department of Veterans Affairs (VA): VA National HIV/AIDS Website; For Veterans and the Public
- U.S. Department of Health and Human Services (HHS): HIV/AIDS Basics
- Centers for Disease Control and Prevention (CDC):
- National Institute of Allergy and Infectious Diseases (NIAID/NIH): What Are HIV and AIDS?
HPV
Human papillomavirus or HPV is the most common viral sexually transmitted disease (STD) in the United States. According to the Centers for Disease Control and Prevention (CDC), at least one out of every two sexually active people will have HPV at some point in their life.
There are over 100 known types of HPV
About 40 types can infect female and male genital areas. Genital HPV are grouped into two types:
- Low-risk types of HPV can cause genital warts or may be completely harmless.
- High-risk types of HPV increase the chances for some types of cancer, like cervical cancer.
How is it spread?
HPV is spread by skin-to-skin contact. Women get HPV from sexual contact with someone who has it. HPV can be spread by vaginal, anal, oral or handgenital sexual contact. Someone who is infected but has no visible signs can still spread HPV to others. People can be infected with more than one type of HPV. Long-term sexual partners with HPV often have the same HPV types.
Most sexually active men and women get genital HPV at some time in their lives.
There is an increased risk of genital HPV infection if you:
- Become sexually active at an earlier age
- Have multiple sexual partners
- Smoke
- Have an immune system that does not work well due to a medical condition (e.g., cancer, HIV/AIDS) or from a medicine that weakens the immune system
What are signs of HPV in women?
Most HPV infections have no signs that can been seen or felt. You can have HPV even if years have passed since you had sexual contact with an infected person. You may never know which sexual partner gave you HPV. HPV infection may cause:
- Genital warts (infection with low-risk viruses)
- Cancer (infection with high-risk viruses)
- Cervical cancer (more common)
- Cancers of the vagina, vulva, anus, throat, tongue or tonsils (less common)
How do you know if you have HPV?
Most women with HPV have no signs of infection. Since most HPV infections go away on their own within two years, many women never know they had an infection. Some HPV infections cause genital warts that can be seen or felt. The only way to know if you have HPV is to ask your health care provider to do an HPV test. Your health care provider may also examine you for other infections.
High-risk types of HPV infection can cause cervical cancer. To detect changes in the cervix caused by HPV, all women should get regular Pap tests. You should talk to your health care provider about when to start, how often, and when to stop having Pap tests.
Pap tests:
- Screen for cervical cancer and changes in the cervix that might turn into cancer
- Are done by a health care provider who collects a cell sample from the cervix with a small brush
- Can find abnormal cells on the cervix caused by HPV
- Can be done with an HPV test if:
- You are age 30 or older.
- You have had an abnormal Pap test result. This will show if HPV caused the changes.
- Should be done within three years of first sexual contact or starting at age 21
- Are important, as treating pre-cancer changes on the cervix can prevent cervical cancer
All women, aged 21 and older, should have regular Pap tests.
How is it treated?
Although genital HPV infections are very common, most show no signs and go away without treatment within a few years. If HPV does not go away, treatments are different for low risk HPV and high-risk HPV:
- Low-Risk HPV (Genital warts) – Even when genital warts are treated, HPV infection may remain. Warts can also come back after treatment. Over-the-counter treatments for other types of warts should not be used. Treatments for genital warts include:
- Watch and wait to see if the warts stay the same, get bigger, or go away
- Medicines put directly on the warts
- Burning off the warts
- Freezing off the warts
- Cutting the warts out
- Using special lights or lasers to destroy the warts
- High-Risk HPV – Pap tests can find pre-cancer changes in the cervix and other abnormal cells. Removing the abnormal cells is the best way to prevent cervical cancer.
- Abnormal cells can be surgically removed without removing the uterus or damaging the cervix. After, women can still have normal pregnancies.
What can happen if you have HPV for a long time?
Certain types of low-risk HPV can cause genital warts. Without treatment genital warts may:
- Go away
- Remain unchanged
- Increase in size or number
See Genital Warts for more information.
High-risk HPV can cause abnormal cells in the cervix and cancer if not treated. Almost all cervical cancers are thought to be caused by HPV infections. While there are often no signs of early cervical cancer, some signs may include:
- Increased vaginal discharge, which may be pale, watery, pink, brown, bloody, or foul-smelling
- Abnormal vaginal bleeding between menstrual periods, after sex, douching or a pelvic exam
- Longer or heavier menstrual periods
- Bleeding after menopause
- Pelvic pain
- Pain during sex
If you have high-risk HPV the risk of cervical cancer is further increased if you:
- Smoke
- Have had more than three children
- Have used a birth control pill for more than five years
- Have a family history of cervical cancer
- Have limited access to medical testing and care
- Have a suppressed immune system
Almost all cervical cancers are caused by high-risk HPV infection.
If you have HPV
- Get regular Pap tests.
- Discuss treatment and follow-up care with your health care provider.
- Know that partners that have been together for a while often share the same HPV types, even if both have no symptoms.
How can you avoid HPV?
- Get vaccinated against HPV.
- HPV vaccines can protect against 70% of cervical cancers.
- One type of HPV vaccine can protect against the low-risk HPV that causes 90% of genital warts.
- HPV vaccine is recommended for all females 9 to 26 years old.
- The Centers for Disease Control and Prevention (CDC) recommends all 11-12 year old girls and boys get the HPV vaccine.
- Avoid sexual contact.
- Have safer sex:
- Reduce the number of sexual partners.
- Condoms, when used correctly, can reduce the risk of getting HPV. But, condoms may not cover all infected areas. Each time you have sex use a condom (male or female type):
- Before vaginal sex
- Before anal sex
- Before oral sex
- Have sex with only one partner who does not have sex with others and does not have HPV.
- Know that other forms of birth control do not protect against HPV.
Condoms may not fully protect against HPV since HPV can infect areas not covered by a condom.
For more information, see Safer Sex.
What about pregnancy?
Genital warts rarely cause problems during pregnancy and birth. Most women who no longer have visible genital warts do not have problems with pregnancy or birth. If you are pregnant, you should discuss treatment options with your health care provider as the warts may:
- Grow larger and bleed
- Make it difficult to urinate if growing in the urinary tract (rare)
- Make the vagina less elastic during birth if the warts are in the vagina (rare)
- Cause a need for a cesarean section (C-section) birth if the warts block the birth canal (rare)
- Be passed on to the baby during birth (rare)
If you are pregnant and have a HPV infection and an abnormal Pap test, you should discuss your pregnancy with your health care provider.
For more on HPV
- Department of Veterans Affairs (VA): Cervical Cancer: The Power of Early Detection
- Centers for Disease Control and Prevention (CDC):
- National Cancer Institute (NCI/NIH): Understanding Cervical Changes: A Health Guide for Women
- U.S. Department of Health and Human Services (HHS), Office on Women's Health: Human Papillomavirus (HPV) and Genital Warts Fact Sheet
Syphilis
Syphilis is a sexually transmitted disease (STD) caused by bacteria. It has often been called "the great imitator" as so many of the signs and symptoms are like those from other infections.
How is it spread?
Women get syphilis from sexual contact with someone who has it. Anyone who has it can spread it to others. Sometimes sores or infection may not be visible and the person may not know that they have it. Syphilis can be spread between:
- Men and women
- Women and women
- Men and men
Contact with a syphilis sore can spread the infection. It can get into your body through the vagina, anus, mouth and throat, or broken skin. Pregnant women can pass the infection to their babies before they are born.
What are signs of syphilis in women?
There are four stages of syphilis. Each is defined by how long the person has had it. Signs vary in each stage.
- Primary Stage: The first sign of syphilis is often a small, round, firm sore. These appear at the place where it entered the body such as the vulva, vagina, tongue, or lips. These signs may be inside the vagina. Most do not cause pain. There can also be more than one sore. Signs of syphilis often go away in about 3 to 6 weeks even without treatment. If not treated in this stage, it will progress into the other stages.
- Secondary Stage: This stage can start with a rash
over one or more areas of the body. These appear
mostly on the palms of the hands and the bottoms of
the feet. Other signs may be:
- Sore throat
- Swollen glands
- Fever
- Hair loss in patches
- Head and muscle aches
- Weight loss
- Tiredness
- Latent Stage: This stage is also called the hidden stage. It can last many years. Syphilis remains in the body with no signs of infection. After 10 to 20 years without treatment, syphilis can progress to the late stage.
- Late Stage: Syphilis in this stage can cause:
- Numbness
- Problems with blood vessels
- Damage to bones and joints
- Difficulty walking
- Blindness
- Paralysis
- Brain damage
- Dementia
- Heart disease
- Death
How do you know if you have syphilis?
Your health care provider can examine and test you for syphilis. Blood or fluid from a sore can be tested.
How is it treated?
Syphilis can be cured with antibiotics in all stages of the disease. Always finish antibiotic treatment. Do not have sex until after treatment and all signs are gone. See your health care provider if your signs do not go away after finishing treatment. Some damage to your body caused by the disease may remain.
If you have syphilis
- Always finish all antibiotic treatment.
- Do not have sex with someone who has syphilis or has not finished treatment (to prevent re-infection).
- Tell current and recent sex partners of the infection so they can get checked.
- Know that it can raise the risk of getting and spreading HIV.
- Get tested again after 6 and 12 months. Only a health care provider can tell you when you no longer have it.
How can you avoid syphilis?
- Avoid sexual contact.
- Have safer sex:
- Reduce the number of sexual partners.
- Condoms, when used correctly, can reduce the risk of getting syphilis. Each time you have sex use a condom (male or female type):
- Before vaginal sex
- Before anal sex
- Before oral sex
- Have sex with only one partner who does not have sex with others and does not have syphilis.
- Know that other forms of birth control do not protect against syphilis.
For more information, see Safer Sex.
What about pregnancy?
All pregnant women should be tested for syphilis. If you are pregnant and have syphilis, you can pass the infection to your baby during pregnancy or birth. Syphilis during pregnancy can cause:
- Babies with skin sores, blood, liver and other problems
- Miscarriage
- Early birth
- A baby born dead
- A baby that dies soon after birth
Pregnant women and babies born to infected mothers must be treated to avoid problems.
For more on syphilis
- Centers for Disease Control and Prevention (CDC): Syphilis – CDC Fact Sheet
- National Institute of Allergy and Infectious Diseases (NIAID/NIH): Syphilis
- U.S. Department of Health and Human Services (HHS), Office on Women's Health: Syphilis Fact Sheet
Trichomoniasis
Trichomoniasis is an infection caused by a tiny parasite. It affects both men and women. It is also known as "trich".
How is it spread?
Women get trichomoniasis from sexual contact with someone who has it. Anyone who has it can spread it to others. It can be spread between:
- Men and women
- Women and women
- Men and men
Most infected men have no signs of trichomoniasis. Anyone who has "trich" can spread it even if they have no signs of it.
What are signs of trichomoniasis in women?
Some women can have "trich" without having signs. Others have signs that include:
- Increased vaginal discharge that can be foamy, yellow, or yellow-green
- Strong vaginal odor
- Vaginal itching and irritation
- Discomfort during sex or urination
See your health care provider to be tested if you have signs of "trich".
How do you know if you have trichomoniasis?
The only way to know if you have trichomoniasis is by a medical exam. Your health care provider can use a simple vaginal swab to test for it. Your provider may also ask to test you for other infections at the same time. See your health care provider to be tested for trichomoniasis each year if you:
- Are age 25 or younger and are sexually active
- Are older than 25 with new or multiple sex partners
- Do not practice safe sex
- Are having sex with someone who might be having sex with others
- Are pregnant
How is it treated?
Trichomoniasis can be treated and cured with prescription pills. Always finish treatment. Do not have sex until after treatment and all signs are gone. See your health care provider if your signs do not go away after finishing treatment.
If you have trichomoniasis:
- Always finish all treatment.
- Do not have sex with someone who has trichomoniasis or has not finished treatment (to prevent re-infection).
- Tell current and recent sex partners of the infection so they can get checked.
- Know that it can raise the risk of getting and spreading HIV.
How can you avoid trichomoniasis?
- Avoid sexual contact.
- Have safer sex:
- Reduce the number of sexual partners.
- Condoms, when used correctly, can reduce the risk of getting trichomoniasis. Each time you have sex use a condom (male or female type):
- Before vaginal sex
- Before anal sex
- Before oral sex
- Have sex with only one partner who does not have sex with others and does not have trichomoniasis.
- Know that other forms of birth control do not protect against trichomoniasis.
For more information, see Safer Sex.
What about pregnancy?
Trichomoniasis, if not treated, can increase the risk of low birth weight babies or early birth. Tell your health care provider if you have any signs of "trich" so you can be tested. Discuss treatment options with your health care provider.
For more on trichomoniasis
- Centers for Disease Control and Prevention (CDC): Trichomoniasis – CDC Fact Sheet
- U.S. Department of Health and Human Services (HHS), Office on Women's Health: Trichomoniasis Fact Sheet
Hepatitis
Hepatitis means that the liver is inflamed. This inflammation (swelling) can be caused by germs, viruses, some medicines, some diseases, or heavy alcohol use.
Three common types of hepatitis are caused by viruses
- Hepatitis A virus causes hepatitis A.
- Hepatitis B virus causes hepatitis B.
- Hepatitis C virus causes hepatitis C.
These three kinds of hepatitis can be acute. Hepatitis B and C can become chronic.
Chronic hepatitis B and C are serious health problems.
Acute viral hepatitis
- Is caused by hepatitis A, hepatitis B, and hepatitis C viruses
- Usually occurs within a few weeks after you first get infected with the virus
- Can be mild, severe or even life-threatening
- Hepatitis B or C can sometimes lead to long-term (chronic) infection.
Chronic viral hepatitis
- Is caused only by hepatitis B and hepatitis C viruses
- May be lifelong
- Can cause liver damage, cirrhosis (scarring of the liver), and liver cancer
Symptoms can appear anywhere from 2 to 6 weeks after contact with the virus.
What are the signs of hepatitis?
You may not have any sign of hepatitis. Or, you may have:
- Yellow skin or eyes (jaundice)
- Tiredness
- Fever
- Nausea
- Vomiting
- Loss of appetite
- Stomach pain
- Light stools
- Dark urine
Hepatitis A
Hepatitis A is a disease of the liver caused by hepatitis A virus. It may make you sick for a few weeks to a few months. Most recover with no lasting liver damage.
How is it spread?
Hepatitis A is spread by coming in contact with the hepatitis A virus. This includes:
- Contact with any person infected with the hepatitis A virus
- Sexual contact with an infected person
- Touching contaminated surfaces and then placing your hands near or in your mouth
- Sharing eating utensils that have virus on them
- Eating food or drinking water that has been contaminated by feces that contain the virus. The food and drinks most likely to be contaminated are:
- Fruits
- Vegetables
- Shellfish
- Ice
- Water
In the United States, chlorine in the water kills hepatitis A virus. But infected food workers can still spread hepatitis A directly to food. This occurs when hands are not washed or cleaned before food is handled.
Infected people can spread the virus to others a few weeks before they begin to feel bad.
Who is at risk of hepatitis A?
Anyone can get hepatitis A if they have not been vaccinated. In the U.S., you are at a higher risk if you:
- Use illegal drugs, whether injected or not
- Live with someone who has hepatitis A
- Have bleeding problems and take clotting factors
- Have oral-anal sexual contact with someone who has hepatitis A
- Travel to areas that have high rates of hepatitis A
Travel to Africa, Asia, Eastern Europe, or Central and South America, including Mexico, increases the risk of getting hepatitis A.
What are signs of hepatitis A?
Hepatitis A does not always cause people to feel bad. It may make you sick for a few weeks to a few months. Older people can get sicker when they have hepatitis A. Young children with hepatitis A usually do not show any signs. Signs of hepatitis A include:
- Yellow skin or eyes (jaundice)
- Tiredness
- Fever
- Nausea
- Vomiting
- Loss of appetite
- Stomach pain
- Light stools
- Dark urine
- Diarrhea
How do you know if you have hepatitis A?
The only way to know if you have hepatitis A is by a medical exam. Your health care provider can examine and test you for hepatitis A.
How is it treated?
There are no medicines for treating hepatitis A. If you have been exposed to hepatitis A virus, tell your health care provider. They may be able to give you a protein that fights hepatitis A virus to help keep you from getting sick. Most people with hepatitis A recover without treatment in a few months. A few people will need to be hospitalized for hepatitis A.
What can happen if you have hepatitis A for a long time?
People with hepatitis A usually improve without treatment and have no lasting liver damage. Symptoms usually last less than 2 months. A few people can be ill for as long as 6 months. Hepatitis A can sometimes cause liver failure and death. This is usually occurs in:
- People 50 years of age or older
- People with other liver diseases, such as hepatitis B or C
If you have hepatitis A
- Get plenty of rest.
- Eat healthy foods.
- Drink plenty of fluids.
- Avoid drinking any alcohol.
- Check with your health care provider before taking:
- Medicines
- Supplements and herbal medicines
- Over-the-counter drugs
- Clean hands often, especially after using the bathroom.
- Avoid preparing food, if possible, while you are sick.
- Talk to those listed below about having hepatitis A so they can get more information to protect themselves:
- Household contacts
- Sexual contacts
- Playmates/attendees at childcare centers
- Persons sharing illegal drugs
- Persons sharing food or drink
- Coworkers and/or restaurant patrons where there is an infected food worker
If you have hepatitis A, avoid drinking alcohol.
For more on how to clean hands, see Clean Hands.
How can you avoid hepatitis A?
The best way to prevent hepatitis A is to be vaccinated. People with certain risk factors and health problems need this vaccine. Ask your doctor if the vaccine is right for you. You cannot get hepatitis A from the vaccine. Hepatitis A vaccination is recommended for:
- All children at age 1 year
- People who use injection and non-injection illegal drugs
- People with chronic (lifelong) liver diseases, such as hepatitis B or hepatitis C
- People with bleeding problems who take clotting factors
- People whose work has a risk for hepatitis A infection
- People who live in areas with high rates of hepatitis A infection
- Travelers to countries that have high rates of hepatitis A. These include:
- Africa
- Asia
- Latin America
- South America
- Eastern Europe
CDC's Travelers' Health site has information about hepatitis A and other vaccines.
Getting vaccinated is the best way to prevent hepatitis A.
Other ways to avoid hepatitis A:
- Boil water or drink bottled water in places where the water may not be clean.
- Eat cooked foods and fruits that you can peel. Avoid eating uncooked vegetables or fruits that could have been washed with dirty water, such as lettuce.
- Avoid eating raw or steamed shellfish such as oysters. Shellfish may live in dirty water.
- Use condoms correctly and every time you have sex.
- Clean hands often.
What about pregnancy?
Hepatitis A vaccine does not contain live virus, so the risk to the baby is expected to be low. However, the safety of hepatitis A vaccination during pregnancy is not known. The risk of the vaccination should be weighed against the risk for hepatitis A in pregnant women. Ask your health care provider if the vaccine is right for you.
For more on hepatitis A
- Department of Veterans Affairs (VA): Hepatitis A Basics
- Centers for Disease Control and Prevention (CDC):
- National Institute for Allergy and Infectious Diseases (NIAID/NIH): Hepatitis
- U.S. Department of Health and Human Services (HHS), Office on Women's Health: Viral Hepatitis Fact Sheet
Hepatitis B
Hepatitis B is a disease of the liver caused by hepatitis B virus. Most adults who have hepatitis B will recover on their own. However, children and some adults can develop chronic (lifelong) hepatitis B.
How is it spread?
Hepatitis B virus is spread by contact with body fluids that carry the virus, such as:
- Blood
- Semen
- Vaginal fluids
- Other body fluids
Hepatitis B is spread by contact with infected body fluids, mostly by:
- Sexual contact: (This is the most common way it is spread in the U.S.)
- Vaginal and anal sex
- Sharing unclean sex toys
- Body fluids with hepatitis B can enter tiny breaks or rips in the linings of the vagina, vulva, rectum,or mouth. Rips and tears in these areas can be common and often unnoticed.
- Needle sharing:
- Used or unclean needles
- During illegal drug or drug equipment use
- Contact with blood:
- Open sores of an infected person
- Sharing items such as razors or toothbrushes with an infected person
- Being tattooed or pierced with tools that were not properly cleaned
- Pregnancy and birth:
- Hepatitis B can spread to babies during pregnancy and birth.
Infected mothers can pass hepatitis B to their babies during childbirth.
Hepatitis B is rarely spread from a blood transfusion because:
- Hepatitis B tests are done on all donated blood.
- Blood and blood products that test positive for hepatitis B are safely destroyed. None are used for transfusions.
- There is no risk of getting hepatitis B when donating or giving blood.
Who is at risk of hepatitis B?
Anyone can get hepatitis B if not vaccinated. However, in the U.S., you may be at a higher risk if you:
- Have sex partners that have hepatitis B
- Have HIV or another STD
- Inject drugs or share needles, syringes, or other drug-injection equipment
- Live with someone who has hepatitis B
- Are undergoing dialysis
- Have diabetes
- Travel to areas that have moderate to high rates of hepatitis B (see: Infectious Diseases Related To Travel: Hepatitis B)
- Work in health care or public safety and are exposed to blood or body fluids on the job
- Are an infant born to an infected mother
What are signs of hepatitis B?
When you first get hepatitis B, it is called acute hepatitis B. Most adults who have hepatitis B will recover on their own. However, children and some adults can develop chronic (lifelong) hepatitis B.
Acute hepatitis B: Signs of acute hepatitis B can appear within 3 months after you get the virus. These signs may last from several weeks to 6 months. Up to 50% of adults have signs of acute hepatitis B virus infection. Many young children do not show any signs. Signs include:
- Yellow skin or eyes (jaundice)
- Tiredness
- Fever
- Nausea
- Vomiting
- Loss of appetite
- Stomach pain
- Light stools
- Dark urine
- Joint pain
Chronic hepatitis B: Hepatitis B is chronic when the body can't get rid of the virus. Children, mostly infants, are more likely to get chronic hepatitis B than adults. People with chronic hepatitis B may have no signs for as long as 20 or 30 years. Signs may be the same as acute hepatitis B. There may also be signs of liver damage and cirrhosis such as:
- Weakness
- Weight loss
- Small, red, spider-like blood vessels on the skin
- Confusion or problems thinking
- Loss of interest in sex
- Swollen stomach or ankles
- A longer than normal amount of time for bleeding to stop
How do you know if you have hepatitis B?
The only way to know if you have hepatitis B is by a medical exam. There are several blood tests your health care provider can use to diagnose hepatitis B. These tests can tell you:
- If it is an acute or a chronic infection
- If you have recovered from infection
- If you are immune to hepatitis B
- If you could benefit from vaccination
How is it treated?
Acute hepatitis B: There are no drugs to treat acute hepatitis B. Doctors usually suggest rest, good nutrition, and fluids. Some people may need to be in the hospital.
Chronic hepatitis B: People with chronic hepatitis B virus infection should receive care from a provider who has experience treating hepatitis B. These providers can be:
- Some internists or family medicine providers
- Infection specialists
- Gastroenterologists (digestive system specialists)
- Hepatologists (liver specialists)
If you have chronic hepatitis B, get checked regularly for signs of liver disease. Discuss treatment with your health care provider. Not every person with chronic hepatitis B needs treatment. If you show no signs of liver damage, your provider will continue to check you for liver disease.
What can happen if chronic hepatitis B is not treated?
Chronic hepatitis B is a serious disease that can result in long-term health problems. Up to 1 in 4 people with chronic hepatitis B develop serious liver problems. These include:
- Liver damage and scarring (cirrhosis)
- Liver failure
- Liver cancer
- Death
If you have hepatitis B
- See your health care provider regularly.
- Tell current and recent sex partners that you have hepatitis B.
- Get plenty of rest.
- Eat healthy foods.
- Drink plenty of fluids.
- Avoid drinking any alcohol. There are ways to help you stop drinking alcohol at: What You Can Do.
- Check with your health care provider before taking:
- Prescription medicines
- Supplements or herbal medicines
- Over-the-counter drugs
- Avoid spreading hepatitis B to others by:
- Having safer sex and using condoms during all sexual contact.
- Not sharing used or unclean needles and sex toys.
- Not donating blood, blood products, or organs.
- Cleaning all blood spills – even those that have already dried. Use a mixture of bleach and water (one part household bleach to 10 parts water). Even dried blood is a risk to others.
- Not sharing personal care items like razors, toothbrushes, nail clippers or earrings.
- Not sharing glucose-monitoring equipment.
- Asking sexual partner(s) and people living in close contact with you to be tested and vaccinated.
How can you avoid hepatitis B?
Getting the vaccine for hepatitis B is the best way to prevent hepatitis B. The hepatitis B vaccine is safe and effective. It is usually given as 3-4 shots over a 6-month period. You will not get hepatitis B from the vaccine. Ask your health care provider if you should get this vaccine. It is recommended for:
- All infants, starting with the first dose of hepatitis B vaccine at birth
- Everyone under the age of 19 who has not been vaccinated
- People whose sex partners have hepatitis B
- Sexually active people who are not in a long-term, faithful relationship
- People with a sexually transmitted disease
- People who share needles, syringes, or other drug-injection equipment
- People who have close household contact with someone infected with the hepatitis B virus
- Health care and public safety workers at risk for exposure to blood or body fluids on the job
- People with kidney disease. This includes all those on dialysis and those being considered for dialysis.
- Adults with diabetes
- Residents and staff of facilities for disabled persons
- People with chronic liver disease
- People with HIV infection
- Travelers to regions with moderate or high rates of hepatitis B (see: Infectious Diseases Related To Travel: Hepatitis B)
Travelers at increased risk for infection include:
- Adventure travelers
- Peace Corps volunteers
- Missionaries
- Military personnel
Certain events may increase the risk for hepatitis B for travelers:
- An injury or illness that requires certain types of treatment. These include anything that breaks the skin such as shots, fluids in the vein, transfusion, stitches, and surgery.
- Dental treatment
- Unprotected sexual contact
- Sharing drug injection equipment
- Tattooing, ear piercing, acupuncture and other practices that break the skin
- Practices with risk for breaking the skin such as manicures and pedicures
- Sharing certain items such as earrings, razors, toothbrushes and nail clippers
The hepatitis B vaccine is the best way to prevent hepatitis B.
Other ways to avoid hepatitis B:
- Avoid sexual contact.
- Have safer sex:
- Reduce the number of sexual partners.
- Condoms, when used correctly, can reduce the risk of getting hepatitis B. Each time you have sex use a condom (male or female type):
- Before vaginal sex
- Before anal sex
- Before oral sex
- Have sex with only one partner who does not have sex with others and does not have hepatitis B.
- Know that other forms of birth control do not protect against hepatitis B.
- Not using or injecting drugs.
- Not reusing or sharing syringes, or drug equipment (works).
- Wear gloves if you have to touch another person's blood.
- Do not use another person's toothbrush, razor, nail clippers or any other item that might have even a tiny bit of blood on it.
- Make sure any tattoos or body piercings are done under good conditions, using:
- Sterile tools
- Clean hands and gloves
- Disinfected work surfaces
For more information, see Safer Sex.
For more on how to clean hands, see Clean Hands.
What about pregnancy?
If you have hepatitis B, your baby has a very high chance of getting it. Pregnant women should be checked for hepatitis B by a health care provider. If you are at risk for hepatitis B, ask your provider about getting vaccinated. The hepatitis B vaccine is safe for pregnant women and their baby. The vaccine can help your baby if:
- It is given to the baby within 12 hours of birth.
- The baby finishes the vaccine series. Note: babies should be tested after the last vaccine shot to make sure they are protected from the disease.
Don't breastfeed until you have discussed it with your health care provider. Avoid breastfeeding if your nipples are cracking or bleeding until the sores heal. Until they heal, you can pump your milk to keep up your milk supply. Do not feed this milk to your baby. Throw it away.
Hepatitis B is a very serious disease for babies. 9 out of 10 babies infected develop chronic hepatitis B.
For more on hepatitis B
- Department of Veterans Affairs (VA): Hepatitis B Basics
- Centers for Disease Control and Prevention (CDC):
- Hepatitis B Information for the Public
- Infectious Diseases Related To Travel: Hepatitis B
- Protect Your Baby for Life; When a Pregnant Woman Has Hepatitis B (609 KB, PDF)
- National Institute of Allergy and Infectious Diseases (NIAID/NIH): Hepatitis
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK/NIH): What I need to know about Hepatitis B
- U.S. National Library of Medicine: Cirrhosis
- U.S. Department of Health and Human Services (HHS), Office on Women's Health: Viral Hepatitis Fact Sheet
Hepatitis C
Hepatitis C is a disease of the liver caused by hepatitis C virus. Hepatitis C infection can lead to chronic viral hepatitis, including liver damage, cirrhosis (scarring of the liver), and liver cancer.
How is it spread?
Hepatitis C virus is mostly spread by blood from an infected person when:
- Sharing needles or other equipment to inject drugs. This is the most common way people get hepatitis C in the U.S.
- Getting a needle stick with a needle that was used on an infected person
- Sharing items that may have come in contact with another person's blood, such as razors, nail clippers, pierced earrings, toothbrushes
- Being tattooed or pierced with tools that were used on an infected person
- Having sexual contact with a person infected with the hepatitis C virus. The risk of getting hepatitis C from sexual contact is thought to be low.
Hepatitis C is rarely spread from a blood transfusion because:
- Hepatitis C tests are done on all donated blood.
- Blood and blood products that test positive for hepatitis C are safely destroyed. None are used for transfusions.
- There is no risk of getting hepatitis C when donating or giving blood.
Hepatitis C is not spread by kissing,hugging, coughing, or sharing food and eating utensils.
Who is at risk of hepatitis C?
Anyone can get hepatitis C. It is important for people at high risk of infection to be tested and treated for hepatitis C. In the U.S., you are at a higher risk if you:
- Have ever used a needle to inject drugs, even if once and long ago
- Had a blood transfusion or organ transplant before 1992
- Are a health care worker who had blood exposure to mucous membranes or to non-intact skin, or a needlestick injury
- Have ever been on kidney dialysis
- Were born of a mother who had hepatitis C at the time
- Are a Vietnam-era Veteran
- Had contact with hepatitis-C-positive blood to nonintact skin or to mucous membranes
- Received tattoos or body piercings in non-regulated settings
- Have ever snorted drugs or shared drug equipment
- Have liver disease
- Have abnormal liver tests
- Have a history of alcohol abuse
- Have hemophilia and received clotting factor before 1987
- Have had a sexual partner with hepatitis C, now or in the past
- Have had 10 or more lifetime sexual partners
- Have HIV infection
The only way to know if you have Hepatitis C is to be tested. VA offers hepatitis C testing and treatment to enrolled Veterans.
What are signs of hepatitis C?
When you first get hepatitis C, it is called acute hepatitis C. About 15% of people who have acute hepatitis C infection clear the virus from their bodies. The other 85% of people develop a chronic (lifelong) hepatitis C infection. Of these, 50 to 80%, if treated, may be cured.
Acute hepatitis C: Most people with acute hepatitis C do not have any signs. If signs occur, the average time is 6-7 weeks after exposure, but can be less or more. Some people can have mild to severe signs including:
- Yellow skin or eyes (jaundice)
- Tiredness
- Fever
- Nausea
- Vomiting
- Loss of appetite
- Stomach pain
- Light stools
- Dark urine
Chronic hepatitis C: 3-5 million persons in the United States have chronic hepatitis C infection. Most people do not know they are infected. They don't look or feel sick until the virus causes liver damage. This can take 10 years or more to happen. Signs may be the same as acute hepatitis C. There may also be signs of liver damage and cirrhosis such as:
- Weakness
- Weight loss
- Small, red, spider-like blood vessels on the skin
- Confusion or problems thinking
- Loss of interest in sex
- Swollen stomach or ankles
- A longer than normal amount of time for bleeding to stop
How do you know if you have hepatitis C?
The only way to know if you have hepatitis C is by a medical exam. There are several blood tests your health care provider can use to diagnose hepatitis C. These tests can tell you:
- If it is acute or chronic infection
- If you have recovered from infection
- If you could benefit from vaccination for hepatitis A and B
In some cases, your health care provider may suggest a liver biopsy. A liver biopsy is a test for liver damage. A needle is used to remove a tiny piece of liver, which is then sent for tests.
How is it treated?
If you have chronic hepatitis C infection, your health care provider will examine you for liver problems and may prescribe drugs to help control the disease. Hepatitis C drugs can help to:
- Clear the virus from the body
- Slow down or prevent liver damage
- Lower the chance of getting cirrhosis and liver cancer
Before starting treatment it is important to discuss your options with your health care provider. Treatment for hepatitis C may not be for everyone. Some patients might not need treatment. Other patients might not be able to be treated due to other medical problems.
What can happen if hepatitis C is not treated?
For every 100 people infected with hepatitis C:
- About 15 will clear the virus from their bodies.
- About 85 will develop chronic (long-term) infection. Of these 85 people:
- 66 will get only minor liver damage
- 17 will develop cirrhosis and may have symptoms of severe liver disease
- 2 will develop liver cancer
Chronic hepatitis C infection is the leading cause of liver cancer and cirrhosis in the U.S. Cirrhosis is scarring of the liver which causes it to not work properly. Both liver cancer and cirrhosis can be fatal. A liver transplant may be necessary if chronic hepatitis C causes the liver to fail.
If you have hepatitis C
- See your health care provider regularly.
- Tell current and recent sex partners that you have hepatitis C.
- Get vaccinated against hepatitis A and hepatitis B.
- Get plenty of rest.
- Eat healthy foods.
- Drink plenty of fluids
- Avoid drinking any alcohol. Alcohol use speeds up the damage hepatitis C causes in your liver. Drinking alcohol before starting hepatitis C treatment makes treatment less likely to work. There are ways to help you stop drinking alcohol at: What You Can Do.
- Check with your health care provider before taking:
- Prescription medicines
- Supplements
- Over-the-counter drugs
- Avoid spreading hepatitis C to others by:
- Having safer sex and using condoms during all sexual contact.
- Not sharing used or unclean needles and sex toys.
- Not donating blood, blood products, or organs.
- Cleaning all blood spills – even those that have already dried. Use a mixture of bleach and water (one part household bleach to 10 parts water). Even dried blood is a risk to others.
- Not sharing personal care items like razors, toothbrushes, nail clippers or earrings.
- Not sharing glucose-monitoring equipment.
- Asking your sexual partner(s) to be tested for hepatitis C (and perhaps other infections).
If you have hepatitis C, you can prevent liver damage by not drinking alcohol and by getting vaccinated for hepatitis A and hepatitis B.
How can you avoid hepatitis C?
Right now there is no vaccination to protect you against hepatitis C. However, you can take steps to protect yourself from becoming infected:
- Don't use injectable drugs.
- If you use drugs, get vaccinated against hepatitis A and hepatitis B and enter a treatment program.
- Never share needles, syringes, water, or "works" for intravenous drug use, to inject steroids, or cosmetic substances.
- Handle needles and other sharp objects safely.
- Do not use personal items that may have come into contact with an infected person's blood.
- Do not get tattoos or body piercings from an unlicensed facility or in an informal setting.
- Wear gloves if you have to touch another person's blood. Always clean hands after removing gloves.
- Have safer sex. Each time you have sex use a condom.
For more information, see Safer Sex.
What about pregnancy?
It is possible to get pregnant if you or your partner has hepatitis C. If you are a pregnant woman who already has hepatitis C (or gets hepatitis C during the pregnancy), the chance of passing the virus to your baby is 4 out of 100. The risk becomes greater if the mother has both hepatitis C and HIV. With good prenatal care, babies born to mothers or fathers with hepatitis C are usually quite healthy. The chance of your baby being infected with hepatitis C is the same whether your baby is born by vaginal delivery or C-section. Before breastfeeding, talk to your health care provider.
For more on hepatitis C
- Department of Veterans Affairs (VA):
- National Institute of Allergy and Infectious Diseases (NIAID/NIH): Hepatitis
- Centers for Disease Control and Prevention (CDC): Hepatitis C Information for the Public
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK/NIH): What I need to know about Hepatitis C
- U.S. Department of Health and Human Services (HHS), Office on Women's Health: Viral Hepatitis Fact Sheet
Bacterial Vaginosis
Bacterial vaginosis, or BV, is a common vaginal infection in women. It is the most common vaginal infection in women of childbearing age, including pregnant women.
While it is not a sexually transmitted disease (STD), some sexual behaviors increase the chances for BV. Women who have never had sex can also have BV.
How is it spread?
The vagina contains many different types of bacteria. Normally, there are large numbers of "good" bacteria that keep the number of "harmful" bacteria very low. Bacterial vaginosis occurs when this balance is upset and there are more "harmful" bacteria than "good" bacteria. The cause of BV is not fully understood.
The risk of BV is higher if you:
- Have a new sex partner or multiple sex partners
- Douche
- Do not use condoms
- Have a female sexual partner with BV
BV is more common in lesbian and bisexual women than in other women. The reason for this is unknown.
What are signs of BV in women?
Women with BV may have few or no signs of infection. Some women with BV have:
- Increased vaginal discharge:
- Often watery
- Gray or white in color
- Sometimes has an unpleasant, fish-like odor, especially after sex
- Itching or irritation in the vaginal area
- Burning during urination
How do you know if you have BV?
BV can be diagnosed during a medical exam. To check for BV, your health care provider looks for signs of infection and collects a sample of vaginal fluid for lab tests.
How is it treated?
BV is treated with antibiotics. These can be in pill form, creams, gels, or ovules. Sometimes BV goes away without treatment.
Female partners of women with BV may need treatment. Male sexual partners do not need treatment
What can happen if you have BV for a long time?
Most often, BV does not cause other health problems. However, if left untreated, BV may increase your risk for:
- Sexually transmitted diseases (STDs) like herpes, chlamydia, gonorrhea, and HIV
- Pelvic inflammatory disease where BV bacteria infect the uterus or fallopian tubes. Pelvic inflammatory disease can cause infertility and increase the risk of ectopic (tubal) pregnancy.
- An infection after a procedure on the female organs. This includes cesarean section, abortion, and surgery on the cervix or uterus.
- Early labor or birth, if pregnant
If you have BV:
- Always finish antibiotic treatment, even if the signs of BV go away
- Talk to female sex partners about getting BV treatment
How can you avoid BV?
Protect the normal balance of bacteria in the vagina by:
- Not douching
- Asking your sex partners to be examined for BV
- Having sex with only one person who only has sex with you
- Using condoms during sex
- Reducing the number of sex partners
- Washing the genital area daily with mild soap and water
For more information, see Safer Sex.
What about pregnancy?
BV is common in pregnant women. Treatment is very important. BV can increase the risk for:
- Low birth weight babies
- Early labor and birth
If you are pregnant and have BV, see your health care provider one month after finishing treatment.
For more on BV see:
- Centers for Disease Control and Prevention (CDC): Bacterial Vaginosis – CDC Fact Sheet
- U.S. Department of Health and Human Services (HHS), Office on Women's Health:
Vaginal Yeast Infections
A vaginal yeast infection is an infection of the vagina and vaginal area. It is caused by a type of fungus called yeast. When this yeast increases it can cause an infection.
Three out of four women will get a vaginal yeast infection during their life. Some women will have it more than once. A vaginal yeast infection is NOT a sexually transmitted disease (STD).
How is it spread?
Yeast is not spread from person to person. Small amounts of yeast can be found in the normal vagina. Infection occurs when too much yeast begins to grow. Vaginal yeast infections can increase with:
- Pregnancy
- Illness such as HIV disease or diabetes
- Some medicines such as:
- Antibiotics
- Birth control pills
- Cortisone-type drugs
- Some chemotherapy drugs
- Stress
- Lack of sleep
- Having your period
Having many vaginal yeast infections may be a sign of other health problems.
What are signs of vaginal yeast infections?
- Itching in the vaginal area
- Vaginal discharge. This is mostly white. It can be watery to thick, and even chunky. It does not have a bad smell.
- Redness, swelling, and burning in the vaginal area
- Pain with urination or during sex
How do you know if you have an infection?
Yeast infections can be diagnosed during a medical exam. To check for a vaginal yeast infection, your health care provider looks for signs of infection and collects a sample of vaginal fluid for lab tests.
How is it treated?
Vaginal yeast infections can be treated with medicines such as pills or creams, ovules, or ointments. Treatment may take from 1 to 7 days days. Women with weak immune systems or other medical problems may need longer treatment. Always finish treatment, even if the signs of a yeast infection go away. Yeast infections can come back if not treated correctly. Infection is more likely to return if some health problems, such as diabetes, are not under control.
What can happen if you don't get treated for a yeast infection?
Signs of infection may get worse without treatment. Scratching the vaginal area can leave open or raw areas. These can become infected with other germs.
How can you avoid vaginal yeast infections?
- Do not douche.
- Avoid scented products such as bubble baths, feminine hygiene sprays, pads or tampons.
- Change pads and tampons often during your period.
- Do not wear tight clothing. This can cause irritation and sweating in the vaginal area.
- Wear cotton underwear.
- Wear pantyhose with a cotton crotch.
- Change out of wet clothing and swimsuits right away.
- Keep blood sugar under control if you have diabetes.
What about pregnancy?
Pregnancy can increase the risk of vaginal yeast infections. Ask your health care provider about safe and effective treatments. Babies born to a mother with a vaginal yeast infection can get a mouth infection (thrush).
For more on vaginal yeast infections
- U.S. Department of Health and Human Services (HHS), Office on Women's Health: Vaginal Yeast Infections Fact Sheet
- U.S. National Library of Medicine: Vaginal Yeast Infection
Urinary Tract Infections
A urinary tract infection (UTI) occurs when bacteria grow in the urinary tract. The urinary tract system makes and stores urine and carries it out of the body.
The organs that can be infected include:
- Bladder (common) – Stores urine
- Urethra (common) – The tube that carries urine from the bladder out of the body
- Kidneys – Collect waste from blood to make urine
- Ureters – Move urine from the kidneys to the bladder
How is it spread?
Women get UTIs more often than men. The risk for UTIs can be increased by:
- Sexual intercourse
- Using a diaphragm
- Conditions that cause urine to stay in the bladder too long
- Problems emptying the bladder completely
- Loss of hormones (after menopause)
- Diabetes
- Kidney stones
- Having a tube that drains urine from the bladder
- Obesity
- Having had several children
UTIs cannot be spread between people.
What are signs of UTIs in women?
UTIs in the bladder and urethra may cause:
- Frequent urge to urinate, but not much urine comes out
- Burning, stinging or pain with urination
- Heavy feeling in the lower belly
- Waking in the night to urinate
Other signs of UTI may include:
- Pain or pressure in the lower back or sides
- Urine that smells bad or looks dark, cloudy, or red
- Tiredness, fever, and chills
How do you know if you have a UTI?
A health care provider can examine you for UTIs. A urine sample will be tested. Other tests may be done if your provider thinks the infection has spread, or if you have had many UTIs. You may be asked about:
- Signs of your UTI
- Past UTIs
- Sexual contact
- Birth control methods
- Pregnancy
- Other health conditions, such as diabetes
How is it treated?
UTIs are treated and cured with antibiotics. Always finish antibiotic treatment. If treated quickly, UTIs usually do not cause serious problems. You may need longer treatment or a different antibiotic if you:
- Are pregnant
- Have frequent UTIs
- Have diabetes
- Have a UTI that has spread to your kidneys
UTIs in the bladder and urethra that are not treated can spread to the kidneys and cause serious illness.
If you have a UTI
- Always finish antibiotic treatment
- Return to your health care provider if:
- Signs don't go away
- Signs come back
- Signs get worse
- You have more or different signs of UTI
Some doctors suggest showers instead of baths, and sanitary pads instead of tampons.
How can you avoid UTIs?
- Urinate when you have the urge.
- Don't hold in urine for a long time.
- Urinate before and after having sex.
- Drink plenty of fluids.
- Clean your genital area every day.
- Avoid the use of douches and perfumed sprays for the genital area.
What about pregnancy?
It is important to notify your health care provider right away if you are pregnant and think you may have a UTI. In pregnant women, UTIs:
- May result in early labor or early birth
- May cause harm to the baby, or even death
- Are more likely to spread to the kidneys
For more on UTIs
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK/NIH): Urinary Tract Infections in Adults
- U.S. National Library of Medicine: Urinary Tract Infection – Adults
- U.S. Department of Health and Human Services (HHS), Office on Women's Health: Urinary Tract Infection Fact Sheet
Safer Sex
Safer sex can help you reduce your risk for exposure to sexually transmitted diseases (STDs). STDs are spread by sexual contact with an infected person. This occurs through vaginal, anal, or oral sex, and genital touching.
What is safer sex?
The only way to be absolutely sure of avoiding STDs is to not have any sexual contact. Having safer sex is one of the best ways to protect yourself from STDs. Safer sex uses barriers to reduce the risk of blood or body fluids entering the body. The most common barrier used is the male condom. Barriers should be used during all sexual contact. Barriers include:
- Male condoms
- Female condoms
- Other barriers
How are barriers used?
Each time you have sex use a barrier to prevent the spread of STDs, including HIV. Barriers can be made of plastic or latex and protect against viral STDs. Use barriers for:
- Vaginal sex
- Anal sex
- Oral sex
Talk to your partner about using barriers:
- Before sex
- Decide on sexual limits that you are both comfortable with
- Remember that alcohol and drugs can alter your judgment about if, when, or how to use barriers
- Decide what type of barrier to use: male or female condoms, or other barriers
- Make sure to have barriers on hand if there is a possibility that you will have sex
Condoms kept in a wallet, stored somewhere warm, or that have been washed in the washer should not be used.
Male condoms
- Use for oral, anal or vaginal sex.
- Choose lubricated latex condoms:
- "Lambskin" or natural condoms do not block HIV or other STDs
- If you have allergies to latex, choose polyurethane (plastic) condoms
- Use before the expiration date.
- Store in a cool, dry place.
- Use a new condom for each sex act, from start to finish.
- Always follow manufacturer's directions for use.
- Carefully open the package, make sure there are no holes in the package.
- Check the condom for rips or signs of damage like brittleness or stickiness.
- Place the condom on an erect penis.
- Partially unroll the condom to find the right side then hold onto the tip of the condom as it is placed on the penis.
- Use a water-soluble lubricant (e.g., ID Glide, K-Y Jelly, Slippery Stuff, Foreplay, Wet, Astroglide) after the condom is put on to prevent the condom from breaking.
- Do not use petroleum jelly, massage oils, mineral oil, cooking oil, body lotions, butter, grease, or hand creams as lubricant. These can weaken condoms.
- Remove the condom after ejaculation, but before the penis gets soft.
- If the condom breaks at any point during the sex act remove it and put on a new one.
- Use on sex toys such as dildos or vibrators that are shared:
- Use new condoms for each partner.
- Clean sex toys after each use.
Both male and female condoms are available without co-pay at the VA pharmacy.
Female condoms
- Use for vaginal sex.
- Different shape than the male condom.
- Made of a plastic called polyurethane.
- Use before the expiration date.
- Store in a cool, dry place.
- Use a new condom for each sex act, from start to finish.
- Carefully open the package, make sure there are no holes in the package.
- Check the condom for rips or signs of damage like brittleness or stickiness.
- Always follow manufacturer's instructions for use.
- Lubricate the vagina before inserting the condom.
- Female condoms are made of polyurethane and are already lubricated.
- Water or oil-based lubricants can be used.
- Put lubricant on the inside and outside of the condom.
- Put the condom on up to eight hours before having sex and before beginning any sexual contact.
- Squeeze the ring of the closed end and insert into the back of the vagina. Keep the open end outside of the vagina, partially covering the lip area.
- If the outer ring slips into the vagina, or if the penis is inserted outside of the condom pouch, remove and replace the condom.
- After sex, remove the condom by twisting the outside ring to trap any fluid before standing up. Throw the condom in the trash.
Other Barriers
Other barriers listed below can also be used to make oral sex safer. These work by reducing contact between blood or fluids and the mouth. Place over the opening to the vagina or anus before oral sex.
- Natural latex sheet
- Cut open condom
- Dental dam
- A piece of latex rubber found at surgical supply stores
- Plastic cling wrap
- Can offer some protection if nothing else is available. Scientific research on this is questionable
For more on safer sex
- Centers for Disease Control and Prevention (CDC): Condom Fact Sheet In Brief
- U.S. Department of Health and Human Services (HHS), Office on Women's Health:
Colds
A cold is an infection of the nose, sinuses, and/or throat almost always caused by a virus. A virus is a type of germ that causes infections. There are more than 200 types of viruses that can cause a cold.
How are colds spread?
The most common way to get a cold is by contact with a person who has a cold. A cold virus spreads easily. For example: when a person with a cold sneezes, coughs, talks, or laughs, the virus can spread into the air as droplets from their mouth or nose. These droplets can spread to people as they breathe and to surfaces within 6 feet. Cold viruses can spread to your hands if you touch anything that has the virus on it. If you then touch your eyes, nose, or mouth, you can get infected with cold virus.
What are signs of a cold?
- Stuffy or runny nose
- Sneezing
- Sore throat
- Coughing
- Headache (mild)
- Muscle aches and pains (mild)
- Chest discomfort (sometimes)
- Tiredness (sometimes)
- Fever (rare)
How can you feel better if you have a cold?
- Get plenty of rest.
- Consider the use of over-the-counter drugs, not all over-the-counter drugs are safe for children. Find more on drugs safe to give children at: CDC's Questions and Answers for Parents about Over-the-Counter (OTC) Medicines.
- Use a clean humidifier to help relieve congestion.
- Soothe a sore throat with ice chips, throat spray, or lozenges (do not give lozenges to young children).
- Gargle with warm salt water.
- Do not smoke.
- Avoid second-hand smoke.
If you have a cold
- Clean hands often with soap and water or alcohol hand rub.
- Cough or sneeze into a tissue or into your sleeve.
- Do not share eating or drinking utensils, hand towels, or toothpaste.
- Stay at home if possible.
- Drink plenty of non-caffeinated fluids, such as water, teas, broths, and sports drinks.
- See your health care provider if:
- Your temperature goes over 100.4°F
- Your signs last over 10 days
For more on how to clean hands, see Clean Hands.
How can you avoid a cold?
- Limit or avoid contact with people who are sick.
- Clean hands often.
- Stay healthy. Eat the right foods and get enough sleep.
What about pregnancy?
Pregnant women should not take any over-the-counter drugs for a cold without consulting with their health care provider. If you are pregnant, you may be more likely to get a cold because pregnancy slightly weakens the immune system.
For more on colds
- Centers for Disease Control and Prevention (CDC):
Influenza (Flu)
Influenza or "flu" is a respiratory illness caused by a flu virus. Flu viruses spread each fall, winter, and spring.
Young (infants) and the very old are most at risk for severe illness from seasonal flu. In the U.S., about 3,000 to 49,000 people die yearly from seasonal flu. The Centers for Disease Control and Prevention (CDC) recommends that everyone age 6 months and older get a flu shot each year.
How is it spread?
The flu virus spreads easily. For example, when a person with the flu sneezes, coughs, talks, or laughs, the flu virus can spread into the air as droplets from their mouth or nose. These droplets can spread to people and surfaces within 6 feet.
The flu virus can spread to your hands if you touch anything that has the virus on it. If you then touch your eyes, nose, or mouth, you can get the flu.
The flu virus can live on surfaces, such as countertops and door knobs, for 24 to 48 hours.
Seasonal flu is contagious from 1 day before any signs appear to up to 5 days after you get sick.
Flu spreads easily between people and can live for up to 2 days on surfaces such as doorknobs, tabletops, and counters.
What are signs of flu?
- Fever (usually 102°F or higher)
- Chills
- Cough
- Runny or stuffy nose
- Sore throat
- Tiredness
- Headache
- Muscle or body aches
- Stomach symptoms (mostly in children)
How do you know if you have the flu?
Your health care provider can examine and test you for the flu virus.
How is it treated?
Your health care provider may treat you with antiviral drugs. Antiviral drugs are most effective if taken within the first two days of being sick.
If you have the flu, how can you feel better?
- Get plenty of rest.
- Take over-the-counter drugs. Note: not all over-the-counter drugs are safe for children. Find more on drugs safe to give children at: CDC's Questions and Answers for Parents about Over-the-Counter (OTC) Medicines.
- Use a clean humidifier to help a dry, scratchy throat.
- Soothe a sore throat with ice chips, sore throat spray, or lozenges (do not give lozenges to young children).
- Gargle with warm salt water.
- Eat plain foods that are easy on the stomach.
People with severe illness from the flu should talk to their health care provider about taking antiviral drugs if they get the flu.
What can happen if the flu gets worse?
Most people with the flu will not need medical care or antiviral drugs. Most will recover in less than two weeks. Even healthy people can have severe illness from the flu. Adults should get medical help right away if they develop:
- Difficulty breathing, shortness of breath, or blueish skin color
- Pain or pressure in the chest or abdomen
- Sudden dizziness
- Confusion
- Difficulty waking up
- Severe or continued vomiting
- Flu-like symptoms that improve but then return with fever and worse cough
Over time, flu can lead to:
- Pneumonia
- Bronchitis
- Sinus and ear infections
Illness from flu can also make other health problems worse. People with asthma may have more asthma attacks. People with heart problems may get worse. Flu can cause severe illness and even death in:
- Children younger than 5, especially those younger than age 2
- Adults 65 years of age and older
- Pregnant women
- People who have medical conditions including:
- Asthma
- Diseases of the brain or muscles such as brain injury, muscular dystrophy, cerebral palsy, and stroke
- Chronic lung disease, such as emphysema (COPD) and cystic fibrosis
- Heart disease
- Blood diseases such as sickle cell disease
- Gland diseases such as diabetes
- Kidney diseases
- Liver diseases
- Weak immune systems due to disease or medicines, such as people with HIV/ AIDS, cancer, or those on chronic steroids
- People younger than 19 years of age who are taking aspirin pills long-term
- People who are obese
- American Indians and Alaskan Natives
These people should alert their health care provider if they get signs of the flu. They may need early treatment.
Use this flowchart to help decide how to best handle the flu: Flu Self-Assessment Flowchart (573 KB, PDF).
If you have the flu
- Clean your hands often with soap and water or alcohol hand rub.
- Cough or sneeze into a tissue or into your sleeve.
- Do not share eating or drinking utensils, hand towels, or toothpaste.
- Stay home until 24 hours after their fever is gone except to get medical care or for other necessities.
- Avoid contact with others.
- Drink plenty of fluids, such as water, herbal teas, broths, and sports drinks.
For more on how to clean hands, see Clean Hands.
How can you avoid the flu?
- Get a flu shot each year. Everyone 6 months of age and older should get a flu shot each year because flu virus can change from one year to the next.
- Clean hands and surfaces often.
- Limit or avoid contact with people who are sick.
The best way to avoid the flu is to get a flu shot each year.
What about pregnancy?
Flu can be severe in pregnant women. Get your flu shot. Pregnant women should let their health care provider know if they have any signs of flu. Pregnant women should not take over-the-counter drugs without asking their provider first. The flu shot is safe for pregnant women at any stage of pregnancy.
For more on the flu
- Department of Veterans Affairs (VA): Seasonal Flu
- Centers for Disease Control and Prevention (CDC):
- National Institute of Allergy and Infectious Diseases (NIAID/NIH): Flu (Influenza)
Pneumonia
Pneumonia is an infection of the lungs. Most cases of pneumonia are caused by bacteria (pneumococcal) or viruses (influenza). Rarely, it can be caused by fungi or parasites.
How is it spread?
Pneumonia-causing germs can be spread the same way colds and the flu are spread: into the air as droplets by sneezing, coughing, talking, or laughing. These droplets can spread to people as they breathe and to surfaces within 6 feet.
The germs can spread to your hands if you touch anything that has the germ on it. If you then touch your eyes, nose, or mouth, you can get infected.
Certain people are at a higher risk for pneumonia, including:
- Adults 65 and older
- Children less than 5 years old
- People who smoke
- Alcoholics
- People with lung diseases
- People with a recent cold or the flu
- People who are now or were recently in the hospital
- People who have just had surgery
- People with chronic diseases such as heart disease, liver damage, or diabetes
- People with weak immune systems such as people with HIV/AIDS or certain types of cancer
- People taking drugs which weaken the immune system
- People with problems swallowing, coughing or taking deep breaths
- People with renal failure
- People with sickle cell disease
- People who have had their spleen removed
- People who are living in nursing homes
What are signs of pneumonia?
- Cough (sometimes with thick, creamy, or bloody mucus)
- Fever
- Chills
- Tiredness
- Rapid breathing or shortness of breath
- Chest pain
- Loss of appetite
- Headache
- Nausea and vomiting
How do you know you have pneumonia?
A health care provider can examine you for pneumonia by:
- Asking questions about your symptoms
- Listening to your lungs
- Taking a chest X-ray
- Taking a blood or mucus sampl
More tests may be done if the pneumonia is severe or if you have other health problems.
How is it treated?
- Bacterial pneumonia is treated with antibiotics.
- Viral pneumonia can be treated with antiviral drugs.
Mild cases of pneumonia can be treated at home with medicine and rest. Most severe cases are treated in a hospital. In addition to medicine, oxygen and other methods are used to support breathing and body functions.
What can happen if pneumonia gets worse?
- The lungs cannot send enough oxygen to the body.
- Pus pockets and fluid can form around the lung.
- Infection can spread to other areas of the body.
- In severe cases, pneumonia can cause death.
There are at least 4 million cases of pneumonia every year in the U.S. One out of four will be sick enough to be admitted to a hospital. Adults 65 and older are more likely to be sicker and admitted to a hospital. One out of every 20 cases of pneumonia will be fatal.
Pneumonia causes more deaths than HIV/AIDS.
If you have pneumonia
- Always finish all antibiotic or anti-viral treatment.
- Clean your hands often with soap and water or alcohol hand rub.
- Cough or sneeze into a tissue or into your sleeve.
- Do not share eating or drinking utensils, hand towels, or toothpaste.
- Clean surfaces often such as countertops, refrigerator and freezer handles, doorknobs, and light switches.
- Do not smoke.
For more on how to clean hands, see Clean Hands.
How can you avoid pneumonia?
- Get vaccinated – there are several vaccines (like the flu shot) that can help prevent infection that leads to pneumonia. Talk to your health care provider to see if any of these vaccines are right for you.
- Keep your hands clean with soap and water or alcohol hand rub.
- Limit or avoid contact with people who are sick.
- Keep healthy. Eat the right foods and get enough sleep.
What about pregnancy?
Pneumonia can be more severe if you are pregnant. Tell your health care provider if you have signs of pneumonia during pregnancy. If you are pregnant, check with your health care provider before taking any medicine. Ask your provider which vaccinations you need before you get pregnant, or ones that you need during pregnancy.
For more on pneumonia
- Centers for Disease Control and Prevention (CDC):
- Pneumonia Can Be Prevented – Vaccines Can Help
- Pneumococcal Vaccination
- Podcasts at CDC: Preventing Pneumonia
- U.S. National Library of Medicine: Pneumonia
Vaccines
Vaccines are medical preparations given to help the body produce immunity or to fight disease. Vaccines can prevent outbreaks of disease and save lives. Some diseases are rare in the U.S. as a result of safe and effective vaccines.
You can get vaccinated for many common infections such as
- Influenza
- Hepatitis A
- Hepatitis B
- Human papillomavirus (HPV)
- Streptococcus pneumococcal pneumonia
- Pertussis (whooping cough)
To see which vaccinations you should get, see Vaccinations for Adults (165 KB, PDF).
Are vaccines safe?
Vaccines are some of the safest medical products. But, like any other medical product, there may be risks. Talk to your health care provider about the value of vaccines as well as their side-effects. Vaccines are held to a high standard of safety. In the U.S.:
- Vaccine supplies in the U.S. are the safest, most effective in history.
- Vaccines are monitored for safety and effectiveness.
- Vaccines undergo rigorous and extensive testing.
- Vaccine manufacturers must follow strict production standards.
- The Department of Health and Human Services
(HHS) and three federal agencies primarily work on
vaccine safety:
- Centers for Disease Control and Prevention (CDC)
- National Institutes of Health (NIH)
- Food and Drug Administration (FDA)
- Scientists from FDA and CDC work closely to monitor reports of vaccine side effects (adverse events). The Veterans Health Administration monitors vaccine side effects within its facilities as well.
- Everyone getting a vaccine should receive a Vaccine
Information Statement (VIS) that:
- Explains vaccine benefits and risks.
- Is handed out before each dose of some vaccines.
- Is available in Spanish and other languages at Vaccine Information Statements.
Vaccines are the most effective tool we have to prevent infectious diseases.
Are vaccines effective?
Most childhood vaccines produce immunity about 90-100% of the time. No medicine is perfect, so each vaccine has its own degree of effectiveness. History shows that the number of cases of disease starts to drop when a new vaccine starts to be given.
How do vaccines work with your immune system to prevent disease?
- Vaccines help your body’s immune system prepare to fight germs and infection.
- When vaccinated, your immune system attacks the harmless vaccine and prepares for future "infections".
- When the infection comes along, your body will know how to stop it.
How do vaccines protect you and your community?
Vaccines can prevent disease and save lives. If enough people get vaccinated, large outbreaks of disease can be avoided. Even those not vaccinated get some protection when the spread of contagious disease is contained. This is known as "community" or "herd" immunity. This is true for many diseases, including:
- Influenza
- Measles
- Mumps
- Rotavirus
- Pneumococcal disease
- Pertussis
- Polio
- Rubella
Your health care provider should have a record of all the vaccines have been given. You should also keep a record.
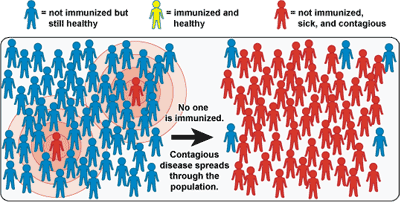
A community in which no one is immunized and an outbreak occurs
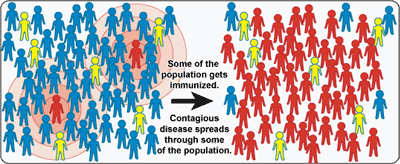
Some are immunized but not enough for herd immunity

Herd immunity – enough people are immunized, protecting most
in the community
Image Source: The National Institute of Allergy and Infectious Diseases (NIAID) at www.vaccines.gov
For more on vaccines
- Centers for Disease Control and Prevention (CDC)
- U.S. Department of Health and Human Services (HHS)
Vaccines and Pregnancy
Discuss vaccinations before, during, and after pregnancy with your health care provider. Many vaccines are beneficial to the health of your baby and yourself.
Vaccination BEFORE pregnancy
Before becoming pregnant, you should be up-to-date on routine adult vaccines. This will help protect you and your child. Discuss vaccines with your health care provider. In general:
- Live vaccines should not be given within a month before getting pregnant or during pregnancy.
- Inactivated (killed) vaccines may be given at any time before or during pregnancy, if needed.
Vaccination DURING pregnancy
If you are pregnant, your health care provider will help you decide which vaccinations you need based on:
- Your age
- Lifestyle
- High-risk conditions
- Type and locations of travel
- Previous vaccinations
To see recommended vaccines for pregnant women, see CDC's Immunization & Pregnancy Flyer (194 KB, PDF) and Immunization & Pregnancy Vaccines Chart (439 KB, PDF).
Vaccination AFTER pregnancy
It is safe for a woman to receive vaccines right after giving birth and when breastfeeding. Vaccines can help protect mothers, including:
- Tetanus, diphtheria and pertussis (Tdap) – if not received during pregnancy
- Measles, mumps and rubella (MMR)
- Varicella (chickenpox)
- Influenza – if not received during pregnancy
While you are pregnant and a short time after the baby is born, your baby has the same immunity and protection from disease that you do. This is temporary. The baby must be vaccinated to develop his/her own immunity.
Your health care provider should have a record of all the vaccines you have been given. You should also keep a record.
Pregnant Women and International Travel
Many diseases, rarely seen in the United States, are common in other parts of the world. A pregnant woman planning international travel should talk to her health care provider about vaccines.
For more on vaccines and pregnancy
- Centers for Disease Control and Prevention (CDC)
- U.S. Department of Health and Human Services (HHS)
Food Safety
The Centers for Disease Control and Prevention (CDC) estimate that every year about 48 million people in the United States become ill from harmful germs in food; of these, about 3,000 die.
What are the signs of illness from food?
- Diarrhea
- Fever
- Vomiting
- Abdominal cramps
- Dehydration
- Death
How is food handled safely?
- Start with food shopping strategies.
- Understand the role of keeping hands, surfaces, and foods clean.
- Learn proper food storage.
- Know proper food thawing.
- Utilize specific preparation techniques.
- Learn how to use a thermometer.
- Recognize serving principles.
- Be prudent when eating out.
You can't see, smell, or taste harmful bacteria that may cause illness.
When shopping for food
- Visit the refrigerated or frozen section last.
- Do not buy food if the package is torn, damaged or leaking.
- Do not buy foods after the "Sell-By" or "Use-By" expiration dates.
Clean hands, surfaces, and foods
- Wash hands thoroughly with water and soap.
- Wash hands before and after handling food, and after using the bathroom, changing diapers, or handling pets.
- Wash cutting boards, dishes, counters, utensils, and hands with hot soapy water after contact with raw meat, poultry, seafood, or unwashed fruits or vegetables.
- Peel or wash fruits and vegetables thoroughly before eating.
For more on how to clean hands, see Clean Hands.
When storing foods you should
- Always refrigerate perishable food within 2 hours (1 hour when the temperature is above 90°F).
- Cook or freeze fresh poultry, fish, ground meats, and other meats within 2 days.
- Cook beef, veal, lamb, or pork, within 3 to 5 days.
- Wrap meat and poultry.
- Wrap meat in the original package with foil or plastic wrap before freezing.
- Store low-acid canned food such as meat, poultry, fish, and most vegetables up to 2 to 5 years.
- Store high-acid canned food such as tomatoes, grapefruit, and pineapples on the shelf for 12 to 18 months.
- Only store cans in good condition, and in a cool, clean, dry place.
- Discard cans that are dented, leaking, bulging, or rusted.
The U.S. Department of Agriculture, Food and Safety Inspection Service has recommendations and information on refrigerator and freezer food storage. Visit: Basics for Handling Food Safely.
When thawing food
- Thaw in the refrigerator.
- Make sure thawing meat and poultry are covered. Keep juices from dripping into or touching other food.
- Refreeze refrigerator-thawed meat and poultry before or after cooking.
- Use cold water for quick thawing if needed.
- Place food in a leak-proof plastic bag.
- Submerge in cold tap water.
- Change the water every 30 minutes.
- Cook immediately after thawing.
- Use a microwave to thaw as needed.
- Cook food immediately after microwave thawing.
The Danger Zone is the temperature that germs can grow in food. Keep food below 40°F or above 140°F (4°C and 60°C).
Check the temperature of your refrigerator and freezer with an appliance thermometer. The refrigerator should be at 40°F or below and the freezer at 0°F or below.
See FoodSafety.gov's Safe Minimum Cooking Temperatures.
When preparing food
- Clean your hands before and after.
- Keep cutting boards, utensils, and countertops clean. Use hot, soapy water and mix with liquid chlorine bleach (1 tablespoon per 1 gallon of water).
- Separate raw meat, poultry, and seafood from ready-to-eat foods.
- Use at least two cutting boards.
- One for raw meat, poultry, and seafood.
- One for fresh fruits and vegetables.
- Don�t let "juice" from foods and packaging touch other foods, utensils, or surfaces.
- Use a clean plate or bowl for cooked food.
- Never use the same plate or bowl that held the uncooked or raw food. Germs from the raw food could get into the cooked food.
- Marinate meat and poultry in a covered dish in the refrigerator.
For more on how to clean hands, see Clean Hands.
When using a thermometer
- Use a food thermometer to check that meat, poultry, and egg dishes reach a safe temperature. Refer to FoodSafety.gov's Safe Minimum Cooking Temperatures or visit: Is It Done Yet.
- Follow the instructions for your food thermometer.
- Place thermometer in the thickest part of the food, not touching bone, fat, or gristle.
- Check at the end of the cooking time, but before the food is expected to be "done".
- Check the temperature in several places to make sure the food is evenly heated.
- Clean your food thermometer with hot, soapy water before and after each use.
- Large-dial oven-safe or oven-probe thermometers may be used during cooking.
- After cooking, allow food to "rest" before cutting or eating. "Rest" times are in FoodSafety.gov's Safe Minimum Cooking Temperatures.
- During the rest time, the temperature of the food will stay the same or rise. This will help destroy harmful germs.
When serving foods
- Keep hot food at 140°F or warmer.
- Keep cold food at 40°F or colder.
- Keep food hot with chafing dishes, slow cookers, and warming trays during parties.
- Keep food cold by nesting dishes in bowls of ice or use small serving trays. Replace them often.
- Don't leave perishable foods out for more than 2 hours at room temperature (1 hour when the temperature is above 90°F).
2 Hour Rule: Keep hot food hot and cold food cold. If food that has been left out is not eaten within 2 hours, discard it.
When eating out
- Choose a clean restaurant. Look for health department reports online or posted in the restaurant.
- Look around you before you sit down. If it's not clean think about eating somewhere else.
- Clean your hands with soap and warm water before eating. If soap and water aren't available, use alcohol hand rub to clean your hands.
- Pay close attention to the type of food and how it's prepared – harmful germs can be hidden in some foods.
- Request that your food be cooked completely through – especially meat, poultry, fish, and eggs.
- Make sure your hot food is piping hot and completely cooked. If lukewarm, send it back.
- Know that raw or undercooked finfish or shellfish (including oysters, clams, and mussels) are more likely to contain parasites or bacteria than foods made from cooked fish.
- Refrigerate take-out and "leftover" food within 2 hours after being served. If you will not be home within 2 hours, don't take the leftovers home with you.
- Bring take-out and "leftover" food directly home after eating out and put your leftovers in the refrigerator as soon as you arrive.
- Eat delivery food within 2 hours after it arrives. This prevents the growth of harmful germs.
If the food is not going to be eaten within 2 hours, you can keep it hot in the oven – but the temperature must be set at or above 200°F (93°C). Side dishes, like stuffing, must also be kept hot in the oven. Covering food will help keep it moist while you keep it warm. Check with a food thermometer to make sure that the inside of the food is held at a temperature 140°F (60°C).
Leftover food should be used within 4 days. Reheat leftovers to 165°F.
For more on food safety
- Department of Veterans Affairs (VA): What Should I Know About Food Safety?
- U.S. Department of Agriculture (USDA), Food and Safety Inspection Service:
Food-borne Illness During Pregnancy
Anyone can get an infection or other type of illness caused by germs or chemicals in foods. Pregnant women are more likely to get a food-borne illness.
It is important for you to learn about food-borne illness before and during pregnancy. Some illnesses caused by food can harm the pregnancy. There are ways to reduce these risks by learning about foods to avoid and how to prepare and handle food carefully.
For both mother and baby, foodborne illness can cause serious health problems – or even death.
What is a food-borne illness?
Some people call this "food poisoning." It is a sickness that occurs when you eat food or drink water that contains harmful substances such as:
- Bacteria
- Parasites
- Viruses
- Certain chemicals
What are the signs of illness from food?
You may get sick very soon after eating contaminated food or symptoms may not occur for days or weeks. This depends on what type of harmful substance is in the food. A food-borne illness can still harm a pregnancy even if the mother does not feel sick. Foodborne illness may cause:
- Fever
- Headache
- Body aches
- Upset stomach
- Diarrhea
- Vomiting
- Abdominal cramps
- Dehydration
- Death
Why are pregnant women at high risk?
- Your immune system is weaker during pregnancy. This makes it harder for your body to fight off harmful germs.
- Your baby's immune system is not fully ready to fight off harmful germs.
- For both mother and baby, food-borne illness can cause serious health problems – or even death.
What foods to eat during pregnancy and what foods to avoid
Certain foods can put pregnant women at a higher risk for food-borne disease. Pregnant women should avoid uncooked meat, poultry and seafood, and unpasteurized dairy products and juices. The table below lists foods to be avoided and ones that are safe to eat.
If you're unsure about the ingredients in a particular dish, ask your server before ordering it. Refer to the table below to find foods safe to eat during pregnancy.
| Food Group | Safe to Eat | Avoid Eating |
|---|---|---|
| Fruits and Vegetables | Washed fruits and vegetables |
Unwashed fruits and vegetables |
Cooked sprouts |
Raw sprouts, such as alfalfa, clover, radish, and mung bean |
|
Pasteurized juice |
Unpasteurized juice |
|
| Dairy | Eggs that are completely cooked |
Eggs that are not fully cooked, runny, without a firm yolk and egg white |
Pasteurized eggs |
Raw unpasteurized eggs |
|
Store bought and pasteurized:
|
Products containing raw unpasteurized eggs including:
|
|
Pasteurized milk |
Unpasteurized milk |
|
Pasteurized cheeses |
Unpasteurized cheeses including:
|
|
| Meat | Hot dogs and lunch meats heated until steaming hot |
Cold hot dogs and lunch meats |
Refrigerated smoked seafood in a cooked dish, like a casserole |
Refrigerated smoked seafood including:
|
|
Fully cooked meats and poultry |
|
|
Pre-stuffed whole poultry that has been purchased frozen and cooked frozen, without defrosting first |
Pre-stuffed poultry that has been purchased fresh and raw |
|
| Seafood | Up to 12 oz. a week (2 average meals) of fully cooked fish with low levels of mercury*, including:
Up to 6 oz. a week of albacore (white) tuna or tuna steaks, which have more mercury than canned light tuna |
Fish with high concentrations of mercury*:
Raw fish, found in foods such as sushi and sashimi |
Fully cooked shellfish |
Raw shellfish including:
|
* Mercury is a harmful metal found in high levels in some fish. Bigger and older fish usually have high levels of mercury. Unborn and newborn babies are more sensitive to mercury than adults. Pregnant and breastfeeding women should avoid fish with high levels of mercury. Pregnant women should eat a variety of fish with low levels of mercury, up to 12 oz. a week. The FDA has more information on mercury in fish and shellfish at: What You Need to Know About Mercury in Fish and Shellfish.
For more information on food safety, visit Food Safety.
For more on food diseases and food safety during pregnancy
- U.S. Department of Agriculture (USDA)
- Centers for Disease Control and Prevention (CDC)
- Food and Drug Administration (FDA)
- U.S. Department of Health and Human Services (HHS): Safe Minimum Cooking Temperatures
Listeriosis
Listeriosis is a food-borne illness caused by bacteria called Listeria. Infected animals can spread these bacteria in their milk and cheese, and to the soil. This can infect animals, vegetables, and other foods that contact soil and animal manure.
How is listeriosis spread?
Listeriosis is spread by eating food or drinking fluids contaminated with these bacteria.
Anyone can get listeriosis, but you are at a higher risk if you:
- Are pregnant
- Pregnant women get listeriosis about 13 times more often than other healthy adults.
- Newborn babies are at risk for more serious illness if infected.
- Are an adult over age 50
- Have a weakened immune system, caused by:
- AIDS
- Cancer
- Diabetes
- Kidney disease
- Medicines for organ transplants and other serious medical conditions
What are signs of listeriosis?
You may have no signs. Or, you may have flu-like signs such as:
- Fever
- Chills
- Muscle aches
- Diarrhea
- Upset stomach
If the illness gets worse, you can have:
- Headaches
- Stiff neck
- Confusion
- Loss of balance
- Convulsions
How do you know if you have listeriosis?
The only way to know if you have listeriosis is by a medical exam. Your health care provider can examine and test for it. Lab samples may be taken from amniotic fluid, blood, feces, and urine.
How is listeriosis treated?
Listeriosis can be treated and cured with antibiotics. Always finish antibiotic treatment.
What can happen to pregnant women if they are not treated for listeriosis?
Listeriosis can be very serious for the pregnant woman and for her child. Listeria bacteria can pass from a pregnant woman to her unborn child. Listeriosis can cause:
- Miscarriage
- Early birth
- Birth of an infected baby
- Brain damage or other problems in the baby
- Death of both the mother and the baby
How can you avoid listeriosis?
- Learn how to handle food safely. This can reduce the risk of listeriosiss and other food-borne illness for you and your family.
- Avoid non-pasteurized soft cheeses.
- Cook food thoroughly.
Pregnant women should avoid eating soft cheeses, deli meats, and cold salads from salad bars.
For more on listeriosis
- Centers for Disease Control and Prevention (CDC)
- Listeriosis (Listeria infection), including information on listeriosis and pregnancy
- U.S. Department of Health and Human Services (HHS), Office on Women�s Health: Food Don'ts; Print-and-Go Guide (126 KB, PDF)
- U.S. National Library of Medicine: Listeriosis
Toxoplasmosis
Toxoplasmosis is an infection caused by a small parasite. It is found in humans, animals, and birds. Cats play a role in the spread of toxoplasmosis.
Cats and kittens can get toxoplasmosis by eating infected small animals. The parasite is then passed in the cat's feces. This can infect their litter box, sand boxes, and soil or dirt in gardens and yards. Kittens and cats can pass millions of parasites in their feces.
How is toxoplasmosis spread?
- Eating undercooked meat (e.g., beef, lamb, pork, poultry, wild game).
- Touching your mouth after:
- Working in infected soil.
- Changing cat litter boxes without wearing gloves. Be sure to clean your hands after.
- Eating fruits and vegetables that are not washed or peeled.
- Handling raw meat without washing your hands afterwards.
- Using unwashed knives, cutting boards, and surfaces that have been in contact with raw meat or other food.
- Drinking water that is infected with the parasite.
Eating undercooked meat is the biggest risk for toxoplasmosis. See FoodSafety.gov's Safe Minimum Cooking Temperatures for safe minimum temperatures for cooking meat.
What are the signs of toxoplasmosis?
You may have no signs of sickness. Or, you may have:
- Muscle aches and pains
- Headache
- Fever
- Sore throat
- Enlarged lymph nodes
- Feel like you "have the flu"
If you are pregnant and have no signs of the illness, your unborn baby can still be affected.
How do you know you have toxoplasmosis?
The only way to know if you have toxoplasmosis is by a medical exam. Your health care provider can examine you and test your blood for it. If a pregnant woman is infected, other tests can show if the unborn baby has toxoplasmosis.
How is it treated?
Toxoplasmosis can be treated and cured with antibiotics. Always finish antibiotic treatment.
What can happen to you if you are not treated for toxoplasmosis?
- Severe cases can affect the brain, lungs, eyes, heart, or liver. Infection can spread to the baby during pregnancy, labor, or birth.
- For the mother, the toxoplasmosis infection is often mild. She may not even know she has it.
- For the baby, infection can cause severe problems.
These are worse when the mother gets the infection
early in pregnancy. Infection of the baby may:
- Cause early birth.
- Damage the baby's eyes, nervous system, skin, and ears.
- Not show for months or years. If not treated, eye or brain problems can occur.
For more on how to clean hands, see Clean Hands.
How can you avoid toxoplasmosis?
- Learn how to handle food safely. This can reduce the risk of toxoplasmosis and other food-borne illness for you and your family.
- Avoid cat litter. If you have to change litter, wear disposable gloves. Clean your hands well with soap and water after.
- Feed your cat store-bought dry or canned food. Do not feed your cat raw or undercooked meats.
- Keep cats indoors. This will keep the cat from hunting birds and rodents that might be infected.
- Avoid stray cats and kittens.
- Do not get a new cat while you are pregnant.
- Keep all sandboxes covered. This will stop cats from using them as litter boxes.
- Wear gloves when gardening or during contact with soil or sand. Clean hands well after gardening or contact with soil or sand.
For more on toxoplasmosis
- Department of Veterans Affairs (VA): Toxoplasmosis
- Centers for Disease Control and Prevention (CDC)
Clean Hands
Keeping your hands clean is one of the best ways to prevent the spread of germs and infection. Clean your hands using soap and water. Or, an alcohol hand rub can be used when your hands are not visibly dirty.
Germs can be spread from your hands to items around you such as doorknobs, grocery carts, handrails, phones, and computer keyboards. After, others may touch these items and then touch their eyes, nose, or mouth. This is just one way that germs pass from one person to another. Keeping your hands clean helps you:
- Avoid getting sick.
- Avoid spreading germs to others.
- Keep your family and community healthy.
- Be a healthy role model for others.
When should you clean your hands?
Before:
- Preparing or eating food.
- Caring for someone who is sick.
- Treating a cut or wound.
- Putting in contact lenses.
After:
- Going to the bathroom.
- Contact with body fluids such as blood, vomit, or feces.
- Changing diapers or helping someone with toileting.
- Caring for someone who is sick.
- Blowing your nose.
- Coughing or sneezing.
- Touching an animal or handling their toys or waste.
- Handling garbage, trash cans, or drains.
- Treating a cut or wound.
- Handling raw meat.
Simply put: Clean your hands often, whether they look dirty or not.
How should you clean your hands?
You can clean your hands using soap and water. Or, you can use an alcohol hand rub (same as alcohol hand sanitizer).
With soap and water:
- Wet your hands with clean running water.
- Add soap to make suds and scrub all over your hands and wrists.
- Rub:
- Palms
- Back of hands
- Between the fingers
- Fingers
- Wrists
- Continue rubbing hands for at least 20 seconds.
- Rinse hands well under running water.
- Dry your hands using a clean paper towel or air dryer. If possible, use your paper towel to turn off the water and to open the door when leaving the restroom.
Need a hand washing timer? Sing "Happy Birthday" through twice in your head!
With alcohol hand rub (alcohol hand sanitizer):
- Apply product to the palm of one hand (see product label for directions/enough to use on BOTH hands).
- Rub:
- Palms
- Back of hands
- Between the fingers
- Fingers
- Wrists
- Keep rubbing until hands are dry, at least 30 seconds.
Most alcohol hand rubs from grocery or drug stores contain alcohol to reduce or kill most germs and viruses. Alcohol hand rubs come in all sizes – even ones that fit in a child's pocket.
Use soap and water instead of alcohol hand rub:
- When your hands are visibly dirty
- Before eating or preparing food
- After handling raw meat
- After handling animal waste
- After going to the bathroom
- After changing a diaper
- After assisting someone with toileting
How can you help others to clean their hands?
- Lead by example and clean your own hands often.
- Teach your friends and family when and how to keep their hands clean.
- Make alcohol hand rub convenient to use. Keep it in places around you such as work, home, and your car. Teach your family and friends to do the same.
- Teach your children good hand cleaning habits, like cleaning their hands before touching their eyes, nose, or mouth.
One way to remind everyone of when to clean hands is to put a bottle of alcohol hand rub next to each box of tissues in your home.
If you are a patient or a visitor in a hospital or medical facility
- Clean your hands and ask your family to do
the same:
- Before entering a patient room or touching a patient.
- After leaving a patient room or touching a patient.
- See staff cleaning their hands with an alcohol hand rub or soap and water before and after they touch a patient.
- See staff putting on gloves before touching broken skin or open wounds.
- See alcohol hand rub in hallways or near patient rooms.
- Ask doctors, nurses, and other staff about the steps the hospital is taking to help staff keep their hands clean.
- Ask or remind hospital staff to clean their hands before and after touching a patient.
Don't be afraid to ask anyone, including health care providers, to clean their hands before touching a patient.
For more on clean hands
- Department of Veterans Affairs (VA): Infection: Don't Pass It On
- Centers for Disease Control and Prevention (CDC)
Contact Lens Safety
Safely cleaning and storing your contact lenses is the best way to prevent eye infections. Lenses can collect bacteria, fungi, and other germs if not properly cleaned.
Why should you clean your contact lenses?
Contact wearers are at risk of eye infections since contacts are worn directly on the eye. Eye infections can cause pain, blurred vision, and sometimes even blindness. Proper contact lens cleaning, storing, and hygiene are the best way to keep your eyes healthy.
Replace contact storage cases every 3 to 6 months.
When should you wear contact lenses?
Most types of contact lenses are only worn while awake. Contact lenses should not be worn when:
- Sleeping (some can be worn overnight)
- Showering
- Swimming in the pool or ocean
Some types of extended wear lenses can be worn overnight. Talk to your eye care provider about when to remove contact lenses.
How should you clean and store your contact lenses?
Follow your eye care provider's and manufacturer's instructions for cleaning and storing your contact lenses.
- Always clean hands before touching your eyes and contact lenses.
- Remove the lens and place in the palm of your hand.
- Rub contact lens solution over the surface of the lens for 5 to 10 seconds on each side.
- Rinse lens with a stream of solution to remove bacteria and deposits from the lens.
- Store lenses in the proper storage case with fresh solution.
- After removing lenses from the storage case, rinse case with fresh solution and allow to air dry. Never use tap water to rinse your contact lens case.
- Replace your contact lens storage case every 3 to 6 months.
Discuss with your provider:
- Which contact lens products and solutions to use
- How often to replace your contact lenses
If you wear contact lenses
Always:
- See your eye care provider for regular exams.
- Clean hands before touching your eyes and lenses.
- Use fresh, sterile solutions recommended by your provider for lens cleaning and storage.
- Remove your contact lenses and see your eye care provider if your eyes become red, irritated, or if you have problems seeing.
- Contact your provider if you have any problems with your eyes, vision, or lenses.
Never:
- Re-use any lens solutions. Always discard all storage solutions after use. Used solutions can become contaminated with germs that can cause eye infections.
- Expose your lenses to water, including distilled, bottled, tap, lake, or ocean water. Water can contain germs that cause eye infections.
- Use saliva to wet your contact lenses.
- Transfer sterile contact lens solution to another container for later use.
Never expose contact lenses to water.
What are signs of an eye infection?
- Discomfort
- Excessive tearing or mucus
- Unusual sensitivity to light
- Itching
- Burning
- "Gritty" feeling
- Unusual redness
- Blurred vision
- Swelling
- Pain
See your eye care provider immediately if you have signs of an eye infection. Eye infections can be serious and in some cases cause blindness.
Allergies can cause some of the same signs as an eye infection. Allergies usually affect both eyes equally. Some infections may affect only one eye.
For more on contact lens safety
- Centers for Disease Control and Prevention (CDC): Acanthamoeba: Microbial Keratitis
- Food and Drug Administration (FDA)
Definition of Terms
Acute infection
A short-term illness caused by a germ.
AIDS (acquired immune deficiency syndrome)
The late stage of HIV infection. When you have AIDS, your immune system is very weak.
Alcohol hand rub, or alcohol hand sanitizer
A liquid or gel used to clean hands. It contains alcohol to kill germs.
Amniotic fluid
Fluid around an unborn baby in the uterus. Amniotic fluid can be used to test for infections during pregnancy.
Antibiotics
A type of medicine used to treat bacterial infections. Antibiotics do not work on viral infections.
Antiviral drugs
A type of medicine used to treat viral infections such as influenza (flu) and HIV.
Bacteria
A type of germ that may cause infection. Not all bacteria are harmful or cause infection. Most bacterial infections are treated with antibiotics.
Bacterial vaginosis (BV)
A common vaginal infection in women that occurs when the balance
of normal bacteria in the vagina is upset. It is the most common
vaginal infection in women of childbearing age. It is also common in
pregnant women.
Biopsy
The removal of a small piece of an organ or tissue to look for signs of disease or damage.
Bladder
The organ in the urinary tract that stores urine.
Cervix
The opening to the uterus (womb).
Chronic infection
A long-term illness caused by a germ.
Chlamydia
A common sexually transmitted disease (STD) caused by bacteria. It can
lead to unusual vaginal discharge and can be harmful during pregnancy. It
may also cause problems getting pregnant.
Cirrhosis
Scarring of the liver.
Cold
An infection of the nose, sinuses, or throat caused by a virus.
"Community" or
"Herd" Immunity
Disease prevention that occurs when most people have been vaccinated
against or have had an infection. This stops the spread of a contagious
disease to protect even those not vaccinated to avoid large outbreaks
of disease.
Condom, female
A plastic barrier inserted into the vagina before intercourse to reduce the
risk of sexually transmitted diseases (STDs) and pregnancy.
Condom, male
A latex, "lambskin", or plastic barrier used to cover the penis during vaginal,
anal, or oral sex to reduce the risk of sexually transmitted diseases (STDs)
and pregnancy.
Contagious
The spread of germs from one person (or other living organism) to another.
Dental dam
A square piece of latex (rubber) or silicone used as a barrier during oral sex
to reduce the risk of sexually transmitted diseases (STDs).
Diaphragm
A type of birth control that is inserted into the vagina to cover the cervix. A
diaphragm does not protect against sexually transmitted diseases (STDs).
Douching
Cleaning or washing the inside of the vagina with water or a mixture
of fluids. The American College of Obstetricians and Gynecologists
recommends that women do not douche.
Fallopian tubes
The tubes that carry eggs from the ovaries to the uterus.
Fungus (fungi)
A type of organism that may cause infection. Fungi can cause vaginal
yeast infections and severe diseases like pneumonia in people with weak
immune systems.
Genital warts
Small growths on the skin in the genital areas that include the penis, vulva,
urethra, vagina, cervix, and around and in the anus caused by human
papillomavirus (HPV).
Gonorrhea
A sexually transmitted disease (STD) caused by bacteria. Also known as
"the clap" or "the drips". It can lead to unusual vaginal discharge and can be
harmful during pregnancy.
Hepatitis
A swollen (inflamed) liver that can be caused by viral infections, drugs,
diseases, alcohol, and/or toxins.
Herpes
A sexually transmitted disease (STD) caused by two types of herpes
simplex viruses.
HIV (human
immunodeficiency virus)
A virus that attacks and weakens the immune system.
Human papillomavirus (HPV)
The most common sexually transmitted disease (STD) in the United States.
There are over 40 types of HPV viruses that can infect genital, mouth, or
throat areas. Some can lead to genital warts or increase the risk for
cervical cancer.
Immune system
Parts of the body that protect against germs and diseases.
Immunity
The ability of your body to avoid an infection or disease.
Influenza (flu)
A respiratory illness caused by a flu virus.
Intrauterine device (IUD)
A type of birth control inserted into the uterus. An IUD does not protect
against sexually transmitted diseases (STDs).
Kidneys
Organs in the urinary tract that collect waste from blood to make urine.
Listeriosis
An infection mainly caused by eating food contaminated with the bacterium
Listeria monocytogenes.
Lymph nodes
Small organs within the immune system spread throughout the body that
help fight infection.
Ovaries
The organs that hold a woman's eggs.
Ovule
A medicine tablet that is inserted into the vagina to treat infections.
Parasite
An organism that can cause infection. Parasites may cause infections such
as trichomoniasis and toxoplasmosis.
Pasteurization
A heating process often used in milk and cheese production that kills
bacteria and other germs.
Pelvic inflammatory
disease (PID)
An infection of the female reproductive organs, including the uterus and
fallopian tubes. Women with a sexually transmitted disease (STD) are at a
higher risk for PID.
Pneumonia
An infection of the lungs that can be caused by bacteria, virus, fungi,
or parasites.
Safer sex
The use of barriers such as condoms during vaginal, anal, or oral sex to
prevent and control the spread of sexually transmitted diseases (STDs) and
other infections.
Sexually transmitted
disease (STD)
Infection spread by vaginal, anal, or oral sex, and genital
touching. STDs can be caused by bacteria, parasites, or viruses.
Common STDs include chlamydia, HPV, and herpes.
Sexually transmitted
infection (STI)
See sexually transmitted disease (STD).
Syphilis
A sexually transmitted disease (STD) caused by bacteria that can
produce sores on the genitals, vagina, anus, rectum, and even
on the lips and in the mouth.
Toxoplasmosis
An infection caused by a small parasite. It is the leading cause of
death from food-borne illness in the United States. It can be very
harmful during pregnancy.
Trichomoniasis
A sexually transmitted disease (STD) caused by a small parasite.
It can lead to unusual vaginal discharge and can be harmful
during pregnancy.
Ureters
Tubes of the urinary tract that move urine from the kidneys to the
bladder.
Urethra
The tube within the urinary tract that carries urine from the
bladder out of the body.
Urinary tract
The body system that makes, stores, and carries urine out of the
body. Includes the kidneys, ureters, bladder, and urethra.
Urinary tract infection (UTI)
An infection that occurs when bacteria grow in the urinary tract.
Uterus
The womb; the part of the female reproductive system where
babies grow and develop during pregnancy.
Vaccine
A medical preparation given to help the body produce immunity
or to fight disease.
Vaginal yeast infection
An infection of the vagina and vaginal area caused by a type
of fungus called yeast. A yeast infection is not a sexually
transmitted disease (STD).
Virus
A type of germ that causes infections and disease. Influenza (flu),
HIV, and herpes are caused by viruses. Antiviral drugs are used
to treat viral infections.
Yeast
A type of fungus that can lead to infection in the vagina.
Download free viewer and reader software to view PDF, video and other file formats.













 stds.html
stds.html




 food-borne-illness.html
food-borne-illness.html





